If your stomach pain after eating is inconsistent and unpredictable, the cause isn’t random — it’s a threshold problem. Here’s exactly what’s driving it.
The Inconsistency Is the Most Confusing Part
If your stomach hurt after every single meal you’d at least have a consistent problem to investigate. But that’s not what’s happening. Some meals are completely fine. Others wreck you. You can eat the same thing twice and get completely different results. You can’t predict it, you can’t explain it, and every time you think you’ve figured out the trigger it happens again with something that should have been safe.
Inconsistent post-meal stomach pain is actually one of the harder digestive patterns to identify the cause of — precisely because of the inconsistency. But that inconsistency itself is a clue. Here’s what it’s telling you about what’s happening in your gut.
Why Inconsistency Points to Specific Causes
Constant pain after every meal typically points to a structural or ongoing inflammatory issue. Pain that comes and goes — present after some meals, absent after others — points to something variable. And the things that vary between meals are: what you ate, how much you ate, how fast you ate, what time of day it was, how stressed you were, and the current state of your gut microbiome on that particular day.
Understanding which of these variables is driving your inconsistent reactions is the key to fixing them. And usually it’s not just one variable — it’s the combination of several that pushes you over a threshold you stay under on your better days.
Reason 1: You Have a Threshold — And Some Meals Cross It
This is the concept most people with inconsistent gut symptoms are missing — and understanding it changes everything.
Your gut has a tolerance threshold for digestive challenge. On a good day — well slept, low stress, well hydrated, earlier in the day — that threshold is higher. Your digestive system is firing well, enzyme production is adequate, gut sensitivity is lower, and meals that would cause problems on a bad day pass without incident.
On a harder day — poor sleep, high stress, dehydrated, eating late, already fatigued — the threshold drops. The same meal that was fine last Tuesday causes cramping and bloating today because your digestive system is operating at reduced capacity and the same food challenge tips you over the edge.
This is why people with inconsistent gut pain so often feel like they can’t identify a pattern. The food isn’t the only variable. Your gut’s capacity to handle that food on any given day is also a variable — and it fluctuates significantly based on sleep, stress, hydration, time of day, and the accumulated load of what you’ve eaten earlier.
Reason 2: FODMAP Stacking
This is one of the most useful concepts for people with inconsistent gut pain — and one of the least known.
FODMAPs are fermentable carbohydrates found in a wide range of foods — garlic, onions, wheat, certain fruits, dairy, beans, and many others. Each food has a FODMAP threshold — a portion size below which most sensitive people tolerate it fine, and above which symptoms are triggered.
Here’s the critical part: FODMAPs from different foods accumulate. A small amount of onion is fine. A small amount of apple is fine. A small amount of wheat is fine. But if you eat all three in the same meal — or even spread across the day — the total FODMAP load can cross your personal threshold and trigger symptoms even though no individual food would have done it alone.
This explains the maddening inconsistency perfectly. Monday you had pasta with a light tomato sauce — fine. Thursday you had pasta with garlic bread and a side salad with apple pieces — same main ingredient but the FODMAP stack crossed your threshold. The pasta didn’t cause it. The combination did.
If your inconsistent pain follows meals that contain multiple foods from the high-FODMAP list — even in modest individual portions — FODMAP stacking is very likely a major driver. Understanding the full picture of what causes post-meal symptoms puts FODMAP stacking in context alongside the other contributing factors.
Reason 3: Your Enzyme Production Varies Day to Day
Your body’s digestive enzyme production isn’t a fixed constant — it fluctuates based on stress levels, sleep quality, hydration, time of day, and your overall health on any given day. This variability is part of why the same meal causes pain on some days and not others.
On a well-rested, low-stress day your enzyme output is optimal and food gets properly broken down. On a poor sleep, high stress day your enzyme production is suppressed — sometimes significantly — and the same meal gets broken down incompletely, reaches your colon partially digested, ferments, and causes pain.
This is also why post-meal pain is consistently worse later in the day for many people. Digestive enzyme production follows a circadian rhythm — it’s naturally higher in the morning and declines through the afternoon and evening. A meal that causes no problems at lunch produces cramping and bloating at dinner — same food, same portion, different enzyme context.
A digestive enzyme supplement levels this out — providing consistent enzymatic support regardless of what your body is producing that day. Zenwise Health Digestive Enzymes taken with every meal ensures the baseline enzyme capacity is there even on your worst days. 👉 Check the current price on Amazon.
Reason 4: Stress as an Unpredictable Variable
Stress is probably the most powerful and most unpredictable variable in gut pain — and the one most people don’t account for when trying to identify their triggers.
The gut-brain axis means that your psychological state directly affects your gut function — enzyme secretion, gut motility, gut sensitivity, and the intensity of the gastrocolic reflex all change measurably based on stress levels. When you’re calm, your gut handles food well. When you’re stressed, the same food produces significantly more discomfort.
The inconsistency this creates can seem completely random — you ate the same lunch two days in a row and one day was fine, one day was awful. But Tuesday you were relaxed. Wednesday you had a difficult meeting right before eating. That’s enough to explain completely different digestive outcomes from identical meals.
If you track your gut symptoms and also track your stress levels on the same days, the correlation is almost always there once you start looking for it. The gut-brain connection runs deeper than most people appreciate — and addressing the stress variable is a legitimate part of managing inconsistent gut pain, not a dismissal of it.
Reason 5: Portion Size Over a Threshold
Your digestive system has a capacity limit for any given meal. Small and moderate portions of even challenging foods often pass without incident. The same foods in larger portions cross a threshold that overwhelms your enzyme capacity or triggers a stronger gastrocolic reflex.
This is why restaurant meals are often worse than home cooking even when you order something seemingly similar to what you make at home — restaurant portions are frequently significantly larger. A restaurant pasta portion might be twice the size of what you’d serve yourself at home, pushing you over the threshold that a home portion wouldn’t reach.
If you track your worst reactions and notice they cluster around larger meals, restaurant eating, or situations where you ate more than usual — portion size crossing your personal threshold is likely a significant factor.
Reason 6: Your Gut Microbiome Has Good Days and Bad Days
Your gut microbiome isn’t static — it fluctuates daily based on what you ate yesterday, how you slept, your stress levels, and dozens of other inputs. On days when your beneficial bacteria are more dominant, your gut handles fermentation more efficiently and produces less gas and discomfort. On days when harmful bacteria have gotten more of a foothold — after a few days of poor eating, after significant stress, after alcohol — your gut is more reactive and the same food produces more symptoms.
This microbiome variability is one of the deeper explanations for day-to-day gut inconsistency. Your gut environment changes, and that changing environment determines how your gut responds to what you eat.
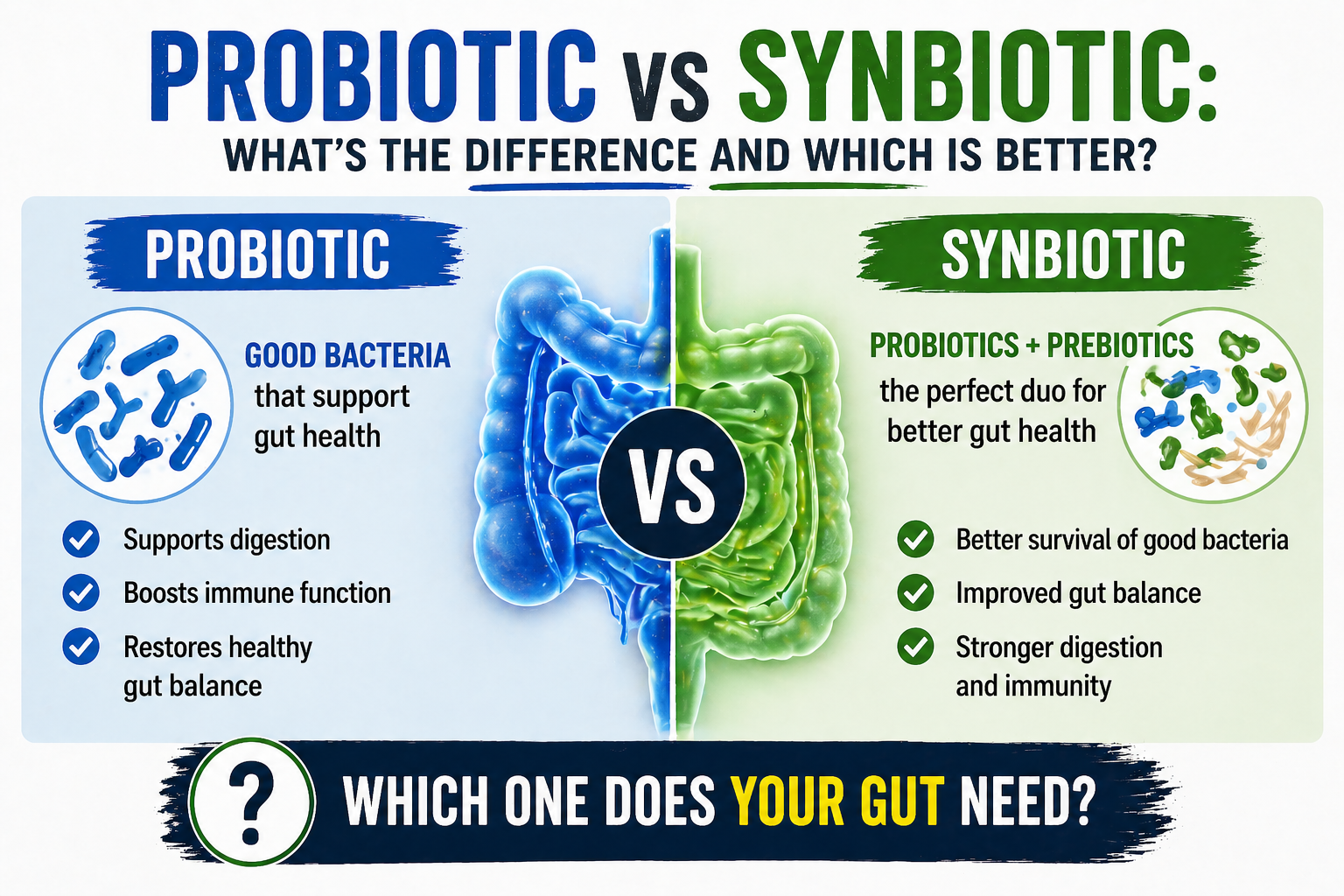
The long-term solution is building a more consistently healthy, resilient microbiome that has less variation — less sensitive on bad days, more capable on all days. A quality synbiotic like Seed DS-01 builds that resilience over 60–90 days of consistent daily use. 👉 Check the current price on Amazon.
How to Figure Out What’s Actually Triggering You
Given the multi-variable nature of inconsistent gut pain, a simple food diary often doesn’t capture enough information to identify patterns. Here’s a more effective tracking approach:
Track more than just food. For each meal note: what you ate, portion size, time of day, stress level (1–10), sleep quality the previous night, hydration, and symptom outcome. Do this for two weeks consistently.
Look for combinations, not single foods. Review your worst symptom days and look for what they have in common — not just which foods were present but which combinations, what time of day, what your stress score was, how you slept. The pattern is almost always more complex than a single food trigger.
Test suspected FODMAP combinations deliberately. If you suspect stacking, try eating your suspected trigger foods individually in moderate portions on separate occasions. If each is fine alone but combinations cause problems, FODMAP stacking is confirmed.
Note how the same food does on high-stress vs low-stress days. This is often the most revealing comparison — if the same food is fine when you’re relaxed and problematic when you’re stressed, the gut-brain axis is the primary variable, not the food itself.
The Practical Protocol
Supplement enzyme production consistently. Since your enzyme production varies day to day and you can’t predict your worst days, taking a digestive enzyme supplement with every meal provides a consistent floor of digestive capacity. This evens out the inconsistency that comes from variable enzyme output. Zenwise Digestive Enzymes daily — one capsule at the start of every meal. 👉 Check the price on Amazon.
Build microbiome resilience for the long term. A healthier, more diverse microbiome has a higher threshold and less day-to-day variability. Daily consistent probiotic use builds that resilience over 60–90 days. Seed DS-01 is our top recommendation. 👉 Check the price on Amazon.
Reduce your baseline FODMAP load. You don’t need to eliminate every FODMAP food — you need to reduce the stack. Identifying your highest-load FODMAP foods and reducing them specifically lowers your daily fermentation baseline and gives you more headroom before symptoms are triggered.
Manage stress around mealtimes specifically. Even if you can’t reduce overall life stress, eating in a calmer state — away from screens, work, and conflict — meaningfully reduces the gut-brain amplification that makes your worst symptom days worse.
Watch portion sizes at dinner especially. Your enzyme output is lowest in the evening and your cumulative daily load is highest. Keeping dinner lighter and avoiding your highest-FODMAP combination foods at dinner reduces the evening threshold crossings that produce your worst nights.
Frequently Asked Questions
Why does my stomach hurt after some meals but not others?
Inconsistent post-meal pain typically reflects a threshold effect — your gut has a tolerance capacity that varies day to day based on stress, sleep, hydration, and time of day. Some meals stay under that threshold, others cross it. The food isn’t always the only variable — your gut’s capacity to handle it on any given day is equally important.
What is FODMAP stacking and could it be causing my symptoms?
FODMAP stacking occurs when multiple foods that are individually tolerable combine in a single meal to exceed your total FODMAP threshold. Each food seems safe alone but the combination triggers symptoms. This is one of the most common explanations for inconsistent gut pain that seems to have no clear single food trigger.
Can stress cause stomach pain after eating some days but not others?
Yes — this is one of the clearest examples of the gut-brain axis at work. The same meal eaten on a high-stress day produces significantly more gut discomfort than the same meal eaten calmly. If your worst symptom days cluster around stressful periods, stress is a major variable in your inconsistency.
Does poor sleep make stomach pain after eating worse?
Yes — sleep deprivation suppresses digestive enzyme production, increases gut sensitivity, and reduces your threshold for symptom triggering. Many people find their gut symptoms are significantly worse the day after poor sleep even when eating the same foods.
Can a probiotic help with inconsistent gut pain?
Yes — by building a more resilient, consistently healthy microbiome that has a higher and more stable threshold. The day-to-day variability in your gut’s behavior is partly a reflection of microbiome instability. A quality probiotic taken consistently over 60–90 days reduces that variability alongside improving overall gut health.
How do I figure out what’s triggering my inconsistent stomach pain?
Track more than just food — include stress levels, sleep quality, time of day, and portion size alongside what you ate. Two weeks of this more comprehensive tracking almost always reveals patterns that a simple food diary misses.
The Goal Is Raising Your Threshold — Not Finding the Perfect Diet
The frustrating thing about chasing inconsistent gut triggers is that you can never fully eliminate the variables. You can’t always control your stress. You can’t always sleep perfectly. You can’t always eat at the ideal time in the ideal portion size.
The better goal — and the more achievable one — is raising your threshold so that normal life variation stops pushing you over it. A healthier microbiome has a higher threshold. Better enzyme support raises your digestive capacity ceiling. Reduced baseline FODMAP load gives you more headroom. Together these don’t eliminate the variables — they raise the point at which those variables start causing symptoms.
That’s what gut health work actually achieves. Not perfection. A gut that handles real life without falling apart.
More from TummyCure:
- Why Am I Bloated After Every Meal?
- Stomach Pain After Eating That Goes Away on Its Own
- Why Does My Stomach Hurt After Eating But Goes Away After Pooping?
- Why Do I Feel Sick After Eating But Not Hungry?
- Why Does My Stomach Hurt After Eating Greasy Food?
- Zenwise Digestive Enzymes — Full Review
- 8 Signs Your Body Needs Digestive Enzymes
- Digestive Enzymes vs Probiotics — Do You Need Both?
- Is Your Gut Sabotaging Your Mental Health?
- The Complete Gut Health Guide
About the Author
Rachel Donnelly is a certified nutritional health coach and gut health writer who spent years struggling with IBS and bloating before making digestive wellness her specialty. She writes for TummyCure with one goal: cut through the noise and tell you what actually works. When she’s not deep in microbiome research, she’s fermenting things in her kitchen and losing arguments with her husband about whether kombucha counts as a dessert.
As an Amazon Associate we earn from qualifying purchases through some links in our articles.