Same Medication, Completely Opposite Gut Reactions — Here’s Why
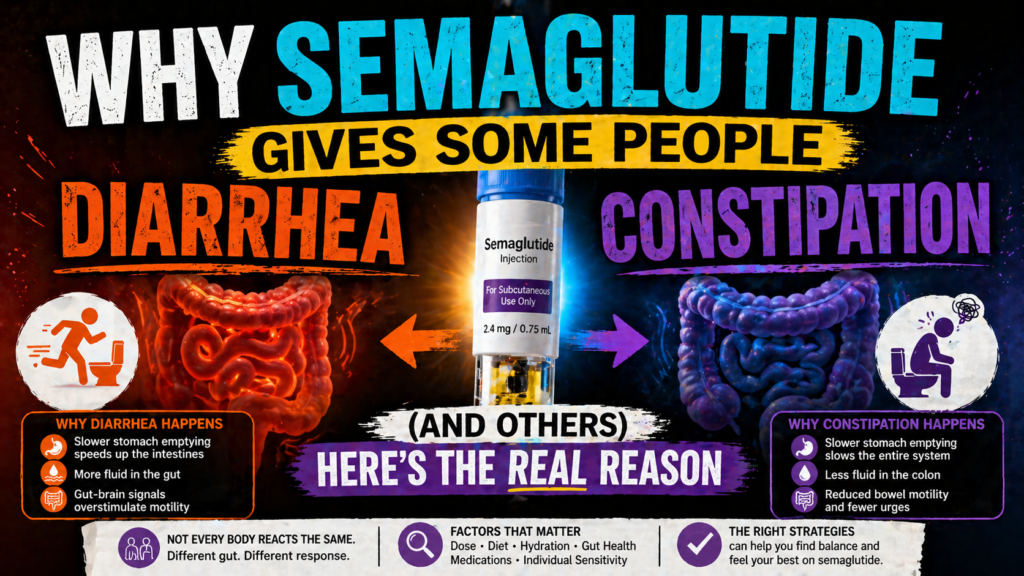
One person starts Ozempic and can’t go to the bathroom for five days. Another starts the same medication at the same dose and is rushing to the bathroom three times before 10am. Both reactions are real, both are common, and both come from the same drug working through the same mechanism.
This isn’t a fluke or a dosing error. It’s one of the most interesting aspects of GLP-1 pharmacology — the way these medications interact with individual gut physiology produces dramatically different bowel outcomes depending on what your baseline gut function looks like, what your microbiome composition is, and how your specific gut responds to altered transit.
Understanding why you got the reaction you did — and what to do about it — starts with understanding how semaglutide actually affects gut motility.
What Semaglutide Does to Gut Motility — The Foundation
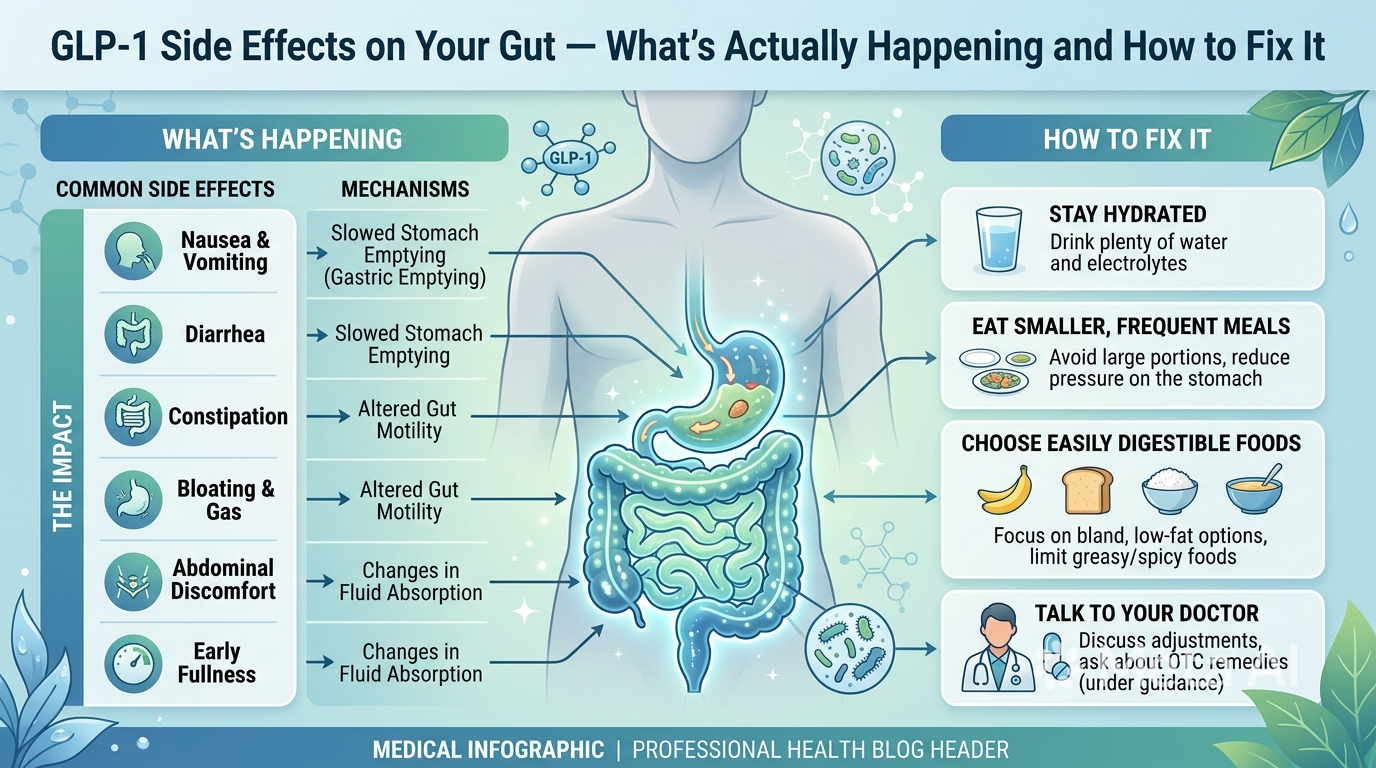
GLP-1 receptors are distributed throughout the gastrointestinal tract — not just in the stomach. Semaglutide activates these receptors comprehensively, producing effects at every level of the digestive system simultaneously. The net effect on any individual’s bowel function depends on how their specific gut responds to this comprehensive receptor activation.
The dominant effect is slowing — particularly in the upper GI tract. Gastric emptying slows significantly. Small intestinal transit slows. This is the intended mechanism for appetite suppression and satiety. In the colon, the picture becomes more complex — GLP-1 receptor activation can either slow or alter colonic motility in ways that produce different effects in different people depending on their baseline colonic function and microbiome composition.
For people whose gut already runs slow — people who were constipated or irregular before starting GLP-1 treatment — the additional motility reduction tips them further into constipation. For people whose gut runs fast — people with IBS-D, a hypersensitive gastrocolic reflex, or a microbiome composition weighted toward motility-stimulating bacteria — the altered motility pattern from GLP-1 can paradoxically produce diarrhea through mechanisms we’ll cover below.
Why Some People Get Constipation on Semaglutide
Constipation is the more common of the two bowel reactions — affecting approximately 20 to 40% of GLP-1 users in clinical data. The mechanism is the most straightforward to understand.
Slowed colonic motility means stool moves through the large intestine more slowly than normal. As stool spends more time in the colon, the colon continues absorbing water from it — that’s its job. The longer stool sits, the more water gets absorbed, the harder and drier it becomes. Hard, dry stool requires more effort to pass, produces incomplete emptying, and builds up over time into the constipation pattern that affects so many GLP-1 users.
Several individual factors make constipation the more likely outcome for a given person:
- Pre-existing slow transit or irregular bowels before starting GLP-1 treatment
- IBS-C history — already prone to constipation-dominant patterns
- Low baseline fiber intake — less material stimulating colonic contractions
- Older age — colonic motility naturally declines with age
- Female sex — women generally have slower colonic transit than men
- Dehydration — GLP-1 thirst suppression makes this very common
- Microbiome weighted toward bacteria that produce fewer motility-stimulating compounds
The complete protocol for managing GLP-1 constipation — magnesium glycinate, psyllium husk, probiotics, hydration — is covered in detail here: GLP-1 Constipation Is Different — Here’s How to Beat It.
Why Some People Get Diarrhea on Semaglutide
Diarrhea affects a smaller but significant proportion of GLP-1 users — approximately 8 to 15% in clinical trial data, with higher rates in the early weeks of treatment and after dose increases. The mechanisms are more complex than constipation and worth understanding specifically.
Fat malabsorption from disrupted lipase timing. This is one of the most underappreciated causes of GLP-1 diarrhea. Normal fat digestion requires coordinated release of bile and pancreatic lipase timed to food arriving in the small intestine from the stomach. GLP-1-slowed gastric emptying disrupts this timing — enzymes and bile may be secreted before food arrives or at suboptimal concentrations relative to the fat load. Incompletely digested fat reaching the colon is a powerful stimulant for urgent, loose bowel movements — this is the same mechanism that produces diarrhea after gallbladder removal or in pancreatic insufficiency.
The overactive gastrocolic reflex. For people with an already-sensitive gastrocolic reflex — the nerve signal from stomach to colon that triggers contractions when food arrives — GLP-1 medications can amplify this response rather than dampen it. The first meal of the day, particularly breakfast combined with coffee, can trigger urgent colonic contractions that produce diarrhea within 30 to 60 minutes of eating. This is identical to the IBS-D morning diarrhea pattern and the morning diarrhea mechanism is directly relevant.
Bile acid spillover. GLP-1 medications alter bile acid metabolism and circulation. Excess bile acids reaching the colon — which can happen when the normal tight coordination between fat digestion and bile secretion is disrupted — act as powerful colonic stimulants producing urgent, watery diarrhea. This is the same mechanism as bile acid malabsorption syndrome and may be more common on GLP-1 medications than currently recognized.
Microbiome disruption producing fermentation imbalance. For people whose gut microbiome is weighted toward rapidly fermenting, motility-stimulating bacterial species, the altered gut environment of GLP-1 treatment can promote proliferation of these bacteria — increasing gas production and accelerating colonic transit toward diarrhea rather than slowing it. The microbiome response to GLP-1 medications is highly individual and depends heavily on baseline composition.
Early weeks dose adjustment response. In the first 2 to 4 weeks of treatment and after each dose increase, some people experience diarrhea as the gut adjusts to the new pharmacological environment before settling into a more stable pattern. This type typically resolves within 4 to 6 weeks at a stable dose without specific intervention.
Why Some People Alternate Between Both
A particularly frustrating subset of GLP-1 users experience alternating constipation and diarrhea — the same unpredictable bowel pattern that characterizes IBS-M. The mechanism is essentially the gut oscillating between overcorrections.
Constipation builds from slowed motility. Eventually the backed-up stool triggers a compensatory colonic response — stronger contractions that produce diarrhea as the backlog clears. After clearing, the slowed motility reasserts itself and constipation begins building again. This oscillating pattern is particularly common in people with pre-existing IBS-M and in people who use stimulant laxatives to treat GLP-1 constipation — the laxative produces overcorrection diarrhea, which then resolves into constipation again.
The management approach for this pattern prioritizes normalizing rather than accelerating or decelerating — soluble fiber like psyllium husk, which has clinical evidence for normalizing transit in both directions, alongside a quality probiotic to stabilize the microbiome composition. The right probiotic for mixed bowel patterns is the same logic applied to the GLP-1 context.
Managing GLP-1 Diarrhea Specifically
If diarrhea is your primary GLP-1 bowel reaction, the management approach differs from the constipation protocol in several important ways.
Digestive enzymes are particularly important. The fat malabsorption and disrupted enzyme timing mechanisms that drive much GLP-1 diarrhea are directly addressed by comprehensive enzyme supplementation. Taking lipase-containing enzymes at the start of every meal ensures fat is properly digested before it reaches the colon to trigger urgent contractions. Zenwise Digestive Enzymes covers lipase alongside a full multi-enzyme blend — for GLP-1 diarrhea specifically this is one of the most directly relevant interventions available. 👉 Check the price on Amazon.
Reduce fat intake dramatically during peak diarrhea periods. Fat is both the trigger for the overactive gastrocolic reflex and the substrate for fat malabsorption-driven diarrhea. Keeping meals very low in fat during the early weeks of treatment and after dose increases reduces the most powerful dietary diarrhea trigger on GLP-1 medications.
Delay or modify morning coffee. Coffee is one of the strongest gastrocolic reflex stimulants available — and for people with GLP-1-related morning diarrhea, the combination of cortisol awakening response, an active gastrocolic reflex, and coffee’s direct colonic stimulation is often the perfect storm that produces the worst morning symptoms. Delaying coffee until after breakfast, switching to half-strength, or eliminating it temporarily during peak symptom periods produces noticeable improvement for many people. Why coffee is particularly hard on sensitive guts in the morning explains the multiple mechanisms at work.
Probiotic support for microbiome stabilization. The bacterial composition underlying GLP-1 diarrhea needs to be addressed at the root. Seed DS-01 includes strains specifically studied for diarrhea regulation alongside broader microbiome support. Give it 6 to 10 weeks of consistent daily use — microbiome-driven diarrhea improvements are gradual but lasting. 👉 Check the price on Amazon.
Soluble fiber — not insoluble. Psyllium husk’s ability to normalize rather than simply accelerate or decelerate transit makes it useful for both constipation and diarrhea — it bulks loose stools while softening hard ones. For GLP-1 diarrhea specifically, starting with one capsule rather than two allows gradual introduction that doesn’t temporarily worsen symptoms. Psyllium husk capsules taken consistently help normalize the bowel pattern from either direction.
Smaller, lower-fat, more frequent meals. Reducing the fat load and volume of any individual meal reduces both the gastrocolic reflex stimulus and the fat malabsorption substrate at a single sitting. The food timing principles that apply to nausea management apply equally to diarrhea management. The food timing strategy for GLP-1 medications is directly relevant.
When GLP-1 Diarrhea Needs Medical Attention
Most GLP-1 diarrhea is self-limiting and manageable with the strategies above. Contact your prescriber if:
- Diarrhea is severe enough to cause dehydration — dark urine, dizziness, significant weakness
- It persists beyond 4 to 6 weeks at a stable dose without improvement
- There is blood in your stool
- Diarrhea is accompanied by significant abdominal pain that doesn’t resolve after emptying
- You’re losing electrolytes to the point of cramping or heart palpitations
- It’s severe enough to be affecting your ability to function normally
Dose reduction is a legitimate clinical option for people whose diarrhea is severe — the bowel effects are dose-dependent and managing symptoms at a lower dose before titrating more slowly is preferable to stopping the medication entirely.
The Individual Factor — Why Your Reaction Is Your Reaction
The most important thing to understand about GLP-1 bowel effects is that your specific reaction reflects your specific gut. Your baseline motility, your microbiome composition, your gastrocolic reflex sensitivity, your fat digestion efficiency — all of these determine which direction your bowel goes when semaglutide enters the picture.
This isn’t random and it isn’t a product defect. It’s personalized gut pharmacology. And it means the management approach needs to be matched to your specific reaction rather than following generic advice that assumes everyone gets the same side effects from the same drug.
If you’re constipated — address the motility reduction directly. If you have diarrhea — address the fat malabsorption and gastrocolic hypersensitivity. If you alternate — normalize rather than push in either direction. The specific protocol differs. The underlying goal is the same: a gut that functions well enough to let you stay on a medication that’s working.
Frequently Asked Questions
Why does Ozempic cause diarrhea in some people and constipation in others?
The net effect on bowel function depends on baseline gut physiology. People with already-slow transit or IBS-C tend toward constipation as GLP-1 further reduces motility. People with sensitive gastrocolic reflexes, IBS-D tendencies, or microbiomes weighted toward fast-fermenting bacteria tend toward diarrhea through fat malabsorption, gastrocolic reflex amplification, and bile acid effects.
Is diarrhea or constipation more common on semaglutide?
Constipation is more prevalent in clinical data — affecting 20 to 40% of users versus 8 to 15% for diarrhea. Both are significant and both deserve specific management approaches.
How long does GLP-1 diarrhea last?
Early-weeks diarrhea from dose adjustment typically resolves within 4 to 6 weeks at a stable dose. Persistent diarrhea from fat malabsorption or microbiome imbalance requires active management and may continue throughout treatment without intervention.
Can digestive enzymes help with Ozempic diarrhea?
Yes — particularly for diarrhea driven by fat malabsorption from disrupted enzyme timing. A lipase-containing multi-enzyme supplement taken at the start of every meal addresses this mechanism directly and produces noticeable improvement for many people with GLP-1 diarrhea.
What should I eat if I have diarrhea on Wegovy?
Very low-fat meals are the highest priority — fat is the strongest dietary diarrhea trigger through both the gastrocolic reflex and fat malabsorption mechanisms. Small, frequent meals rather than large ones. Soluble fiber from psyllium husk to normalize stool consistency. Avoid coffee until symptoms stabilize.
Should I stop Ozempic if I have diarrhea?
For manageable diarrhea — don’t stop. Implement the dietary and supplement strategies above, discuss dose reduction or slower titration with your prescriber if symptoms are significant, and give your body 4 to 6 weeks to adapt at a stable dose. Most GLP-1 diarrhea improves substantially with the right approach and time.
Your Gut Is Telling You How It Works — Listen and Respond
Whether semaglutide gave you constipation, diarrhea, or the frustrating alternation between both — your gut’s response is telling you something specific about your baseline physiology and what it needs. Match the management approach to the reaction. Address the specific mechanisms driving your symptoms rather than applying generic advice designed for a different reaction.
The medication is working. Give your gut the targeted support it needs to work alongside it.
More from TummyCure:
- Complete GLP-1 Gut Side Effects Guide
- GLP-1 Constipation — How to Beat It
- Ozempic Nausea Is a Food Timing Problem
- Why Ozempic and Wegovy Make You So Bloated
- GLP-1 Medications and GERD
- Zenwise Digestive Enzymes — Full Review
- Seed DS-01 — Full Probiotic Review
- Diarrhea Every Morning Then Fine
- Best Probiotic for IBS-C, IBS-D and IBS-M
- The Complete Gut Health Guide
About the Author
Rachel Donnelly is a certified nutritional health coach and gut health writer who spent years struggling with IBS and bloating before making digestive wellness her specialty. She writes for TummyCure with one goal: cut through the noise and tell you what actually works. When she’s not deep in microbiome research, she’s fermenting things in her kitchen and losing arguments with her husband about whether kombucha counts as a dessert.
As an Amazon Associate we earn from qualifying purchases through some links in our articles.