Finished your antibiotics weeks ago but still feeling off? These 8 signs mean your gut microbiome hasn’t finished recovering — and here’s what to do about it.
Finishing the Antibiotics Doesn’t Mean Your Gut Is Done Recovering
Most people assume that once the antibiotic course is finished and the acute infection symptoms are gone, their body is back to normal. The gut doesn’t work that way. Antibiotic-induced microbiome disruption can persist for weeks, months, or in some cases years after the last dose — producing symptoms that seem completely disconnected from the antibiotics you took weeks or months ago.
The tricky part is that post-antibiotic gut dysfunction wears many disguises. Fatigue that you attribute to stress. Skin breakouts you blame on diet. Anxiety that seems to have no obvious cause. Food intolerances that appeared out of nowhere. Most people never connect these symptoms to the antibiotic course they finished six weeks ago.
Here are the most telling signs your gut hasn’t finished recovering — and what to do about each one.
Still experiencing gut symptoms after antibiotics?
Seed DS-01 Daily Synbiotic — 24 clinically studied strains, acid-resistant delivery, prebiotic included. The most comprehensive probiotic for post-antibiotic gut recovery. Start now and continue for 90 days.
👉 Check the current price of Seed DS-01 on Amazon
Sign 1: Your Bowel Habits Still Aren’t Normal
This is the most obvious and most commonly recognized sign of incomplete gut recovery. If your bowel habits were regular before antibiotics and they’ve been irregular, unpredictable, loose, or difficult since — your gut microbiome has not yet rebuilt the bacterial populations that regulate gut motility.
Beneficial gut bacteria — particularly Bifidobacterium species — produce compounds that directly stimulate intestinal contractions and regulate transit time. When these populations are depleted, your gut loses its primary natural motility regulation. The result is the unpredictable, irregular bowel function that makes post-antibiotic recovery so uncomfortable.
If loose stools are your primary symptom, the diarrhea mechanisms covered in why morning diarrhea happens and what drives it apply directly to the post-antibiotic context. If constipation is the issue, why constipation persists despite doing everything right explains the bacterial component that’s most relevant here.
What helps: consistent daily probiotic use — specifically Bifidobacterium-containing formulas — combined with psyllium husk for stool normalization from either direction. Psyllium husk capsules taken daily with a large glass of water normalize transit in both directions — they’re one of the most evidence-backed interventions for post-antibiotic bowel irregularity specifically.
Sign 2: You’re Bloated and Gassy More Than Before
Post-antibiotic bloating is one of the most persistent and most frustrating recovery symptoms. Before antibiotics, your gut processed food with a well-balanced bacterial community that fermented efficiently and produced manageable amounts of gas. After antibiotics, the balance shifts — harmful gas-producing bacteria proliferate in the ecological space cleared by the antibiotic, and the beneficial bacteria that kept fermentation regulated are depleted.
The result is more gas from the same food — more fermentation, more bloating, more discomfort after meals that never caused problems before. If this is your experience weeks after finishing antibiotics, your microbiome has not yet rebalanced its bacterial composition back toward the less gas-producing community you had before.
Digestive enzyme support reduces the amount of undigested food reaching your bacteria — less fermentation substrate means less gas regardless of which bacteria are doing the fermenting. This is one of the most directly effective interventions for post-antibiotic bloating while the microbiome rebuilds.
Reduce post-antibiotic bloating while your gut rebuilds
Zenwise Digestive Enzymes — comprehensive multi-enzyme blend with probiotic and prebiotic. Take with every meal during recovery to reduce the fermentation-driven bloating that incomplete microbiome recovery produces.
👉 Check the current price of Zenwise on Amazon
The full picture of what drives post-meal bloating and what addresses each mechanism: Why Am I Bloated After Every Meal?
Sign 3: Foods That Never Bothered You Before Now Cause Problems
This is one of the most telling — and most underrecognized — signs of incomplete post-antibiotic gut recovery. If dairy, gluten, certain fruits, or other foods that you previously ate without issue are now causing digestive symptoms, your gut barrier has not fully recovered.
Antibiotics deplete the beneficial bacteria that maintain the tight junctions between intestinal cells — the structural proteins that keep your gut lining selectively permeable. When those bacterial populations are depleted, tight junction integrity is temporarily compromised. Food proteins that your gut normally contains and processes without triggering an immune response now cross the gut barrier and create mild inflammatory reactions.
This is the mechanism behind the food sensitivities that commonly develop or worsen after antibiotics — and it’s the same mechanism as leaky gut. How increased gut permeability affects far more than just digestion explains why these new food sensitivities often come with systemic symptoms — fatigue, brain fog, skin reactions — rather than just gut discomfort.
Collagen peptides provide the structural building blocks the gut lining uses to repair tight junctions. Multi collagen peptides added daily to your morning drink directly support this repair process alongside the bacterial repopulation from your probiotic.
Support your gut lining while it repairs
Multi Collagen Peptides — five types of hydrolyzed collagen including types I, III, and IV directly relevant to gut lining tight junction repair. One to two scoops daily in your morning coffee or smoothie.
👉 Check the current price of Multi Collagen Peptides on Amazon
Sign 4: You’re Fatigued Beyond What the Illness Explains
Feeling tired after being sick is expected. Feeling consistently fatigued weeks after the infection has cleared — when you should be back to normal energy — is a sign that incomplete gut recovery is affecting your systemic health.
Your gut microbiome is responsible for producing several B vitamins including B12, B7 (biotin), and vitamin K2. It influences nutrient absorption across the board — when the microbiome is disrupted, you may be eating adequately but absorbing meaningfully less of what you eat. And your gut bacteria directly affect mitochondrial function — the energy-producing machinery in your cells — through the short-chain fatty acids they produce, particularly butyrate.
Depleted Bifidobacterium and Lactobacillus populations mean less butyrate, less efficient nutrient absorption, and measurably lower energy production at the cellular level. The fatigue isn’t just feeling run down — it has a specific biochemical mechanism rooted in incomplete microbiome recovery.
The gut-energy connection is rarely discussed but very real. As the microbiome rebuilds — typically becoming clearly noticeable at the 6 to 10 week mark of consistent probiotic support — energy levels improve alongside the digestive symptoms.
Sign 5: Your Skin Has Broken Out or Worsened
The gut-skin axis is one of the most well-documented connections in gastroenterology research — and one of the most commonly overlooked by people dealing with post-antibiotic skin changes. If your skin has broken out, become more reactive, or developed new sensitivity since your antibiotic course, your gut is very likely the root cause.
Antibiotic-induced gut disruption produces systemic inflammation through two mechanisms: the temporary increase in gut permeability that allows inflammatory compounds into the bloodstream, and the disruption of the bacterial communities that regulate the body’s inflammatory response. Both produce skin-level inflammation that expresses as acne, eczema flares, rosacea, or general skin dullness and irritation.
Ironically, antibiotics are sometimes prescribed for acne — but systemic antibiotics for skin conditions can produce exactly the gut disruption that worsens skin inflammation long-term. The signs that your gut health is directly driving your skin issues covers the gut-skin connection in detail — and post-antibiotic skin worsening is one of the clearest clinical examples of this mechanism.
Rebuilding the microbiome and supporting gut lining integrity — through probiotics, collagen, and anti-inflammatory curcumin — addresses the systemic inflammation at its source. Turmeric curcumin with black pepper reduces the NF-κB mediated gut inflammation that drives both gut and skin symptoms simultaneously.
Sign 6: You’re More Anxious or Foggy Than Usual
Brain fog and anxiety that arrived or worsened after antibiotics and haven’t fully resolved are signs that the gut-brain axis has been disrupted by incomplete microbiome recovery — not signs of a separate psychological problem.
Your gut bacteria produce approximately 90 to 95% of your body’s serotonin and communicate with your brain through the vagus nerve. When Lactobacillus and Bifidobacterium populations are depleted, serotonin production is measurably reduced. Vagal nerve signaling quality declines. The brain receives fewer beneficial signals from the gut and more distress signals from the disrupted bacterial environment.
The result is the cognitive cloudiness, low mood, and anxiety that many people experience post-antibiotics without ever connecting it to their gut. How gut disruption directly affects anxiety and depression covers the full mechanism — and the timeline for mood improvement following microbiome recovery typically runs 6 to 12 weeks of consistent daily probiotic support.
If your mental clarity and mood have been noticeably different since your antibiotic course, this isn’t coincidental — and it won’t fully resolve until the gut-brain axis has been restored through deliberate microbiome rebuilding.
Sign 7: You Keep Getting Sick
Over 70% of your immune system lives in and around your gut — the GALT (gut-associated lymphoid tissue) that lines your intestines is the largest immune organ in your body. Your gut bacteria actively train and regulate your immune cells, helping them distinguish between threats and normal environmental exposures.
When the microbiome is disrupted, immune regulation is disrupted alongside it. The result is an immune system that’s both less effective at fighting genuine threats — making you more susceptible to colds, infections, and illness — and more reactive to normal stimuli — contributing to increased allergic reactions and inflammatory responses. Why over 70% of your immune system lives in your gut explains the immune-microbiome relationship in detail.
If you’ve been getting sick more frequently since your antibiotic course, immune dysregulation from incomplete gut recovery is a very likely contributing factor. The probiotic work that rebuilds the microbiome also directly restores immune regulation — with measurable improvements in immune markers typically appearing at the 8 to 12 week mark of consistent synbiotic use.
Sign 8: Your Symptoms Started After Antibiotics and Never Fully Resolved
This is the broadest and most important sign — and the one most worth reflecting on carefully. If you developed IBS-like symptoms, chronic fatigue, food sensitivities, recurrent skin problems, or persistent anxiety following an antibiotic course — and those symptoms have never fully returned to baseline — post-infectious gut disruption is the most likely explanation.
Post-infectious IBS following antibiotic use is a documented clinical phenomenon. Significant antibiotic-induced microbiome disruption can produce symptoms that persist for years without deliberate intervention — because without active support, some bacterial species may never fully recover to their pre-antibiotic levels. How antibiotics can disrupt your gut for a year or more covers the long-term impact research in detail.
The good news: even long-standing post-antibiotic gut dysfunction responds to active intervention. The timeline for recovery from chronic post-antibiotic disruption is longer than for recent acute disruption, but the same protocol applies — quality synbiotic, prebiotic fiber, fermented foods, gut lining support, and anti-inflammatory dietary choices. Give it 6 months of genuine consistency rather than 90 days if the disruption has been long-standing.
The Complete Recovery Protocol — If You Recognize These Signs
If multiple signs above describe your current experience, your gut recovery needs active support — not passive waiting. Here’s the full daily protocol:
- Seed DS-01 — daily, 90 days minimum. The foundation. 👉 Amazon price here.
- Zenwise Digestive Enzymes — with every meal. Reduces bloating and gas while the microbiome rebuilds. 👉 Amazon price here.
- Psyllium husk capsules — daily with water. Prebiotic fiber and bowel normalization.
- Multi collagen peptides — daily in morning drink. Gut lining structural support.
- Fermented foods — kefir, yogurt, kimchi, sauerkraut — daily throughout recovery.
- Turmeric curcumin with ginger — daily. Gut and systemic anti-inflammatory support.
The full food-based approach to post-antibiotic recovery: Your Gut Recovery Grocery List — What to Eat After Antibiotics
The complete timeline for what’s happening in your gut week by week: How Long Does It Take Your Gut to Recover After Antibiotics?
Frequently Asked Questions
How long does it take for gut to recover after antibiotics?
The most acute symptoms — diarrhea, bloating — typically improve within 1 to 4 weeks. Full microbiome recovery with consistent active support takes 3 to 6 months. Without active support some bacterial species may remain depleted for a year or longer. The complete antibiotic recovery timeline covers this week by week.
Can antibiotics cause long-term gut problems?
Yes — post-infectious IBS and chronic gut dysfunction following significant antibiotic disruption are documented clinical phenomena. Without active microbiome support, some bacterial populations may not fully recover to pre-antibiotic levels, producing ongoing symptoms months or years later.
Why do I still have bloating weeks after antibiotics?
Persistent bloating indicates the gas-producing bacterial populations that proliferated during antibiotic disruption haven’t been displaced by the beneficial bacteria that normally regulate fermentation. Active probiotic support combined with digestive enzymes to reduce fermentation substrate is the most effective approach.
Can antibiotics cause anxiety and depression?
Through the gut-brain axis — yes. Depleted beneficial bacteria produce less serotonin and send fewer beneficial signals through the vagus nerve to the brain. This produces measurably altered mood and cognitive function that resolves as the microbiome recovers. Read more: Can Leaky Gut Cause Anxiety and Depression?
What is the best probiotic for post-antibiotic gut recovery?
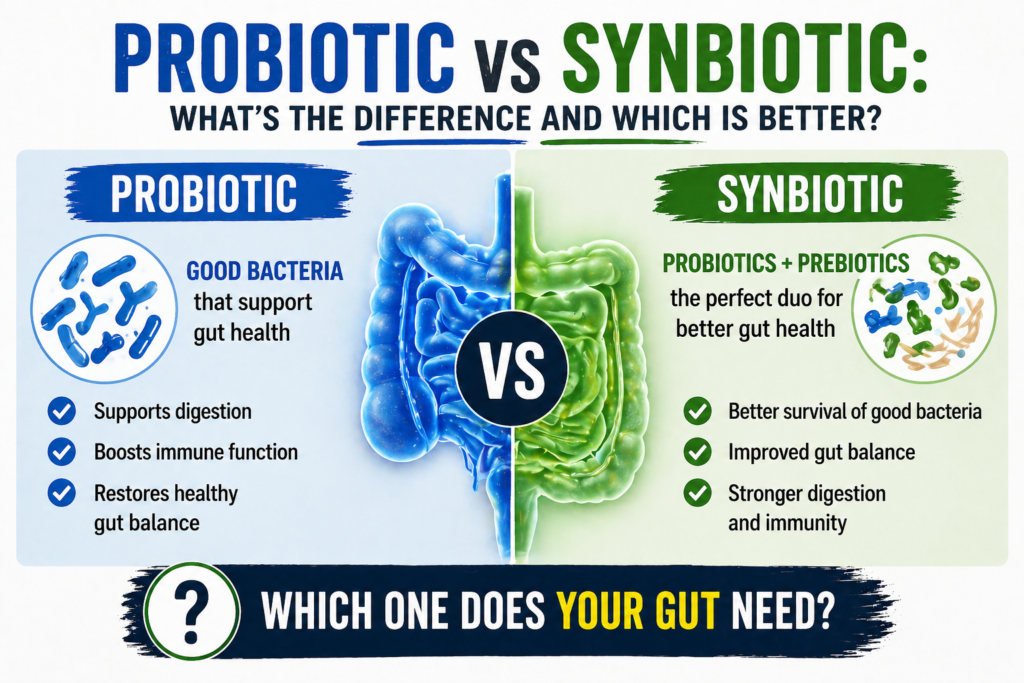
A multi-strain synbiotic with both Lactobacillus and Bifidobacterium strains, acid-resistant delivery, and prebiotic included. Seed DS-01 is our top recommendation. 👉 Check the price on Amazon.
Why do I keep getting sick after antibiotics?
Depleted gut microbiome means depleted immune regulation — over 70% of your immune system is gut-associated. Frequent illness after antibiotics is a sign of immune dysregulation from incomplete microbiome recovery. Rebuilding the microbiome through consistent probiotic use and fermented foods directly restores immune function over 8 to 12 weeks.
Your Gut Is Trying to Tell You It Needs Help — Listen
The symptoms above aren’t random post-illness misfortune. They’re your gut ecosystem communicating clearly that it hasn’t finished rebuilding — and that passive waiting alone isn’t going to get it there. Every week of unaddressed post-antibiotic gut disruption is another week of symptoms that are affecting your quality of life unnecessarily.
The recovery protocol works. The research supports it. Start it today — even if your antibiotic course ended weeks or months ago. Your gut can rebuild from wherever it currently is — it just needs the right consistent support to do it.
Start your gut recovery today — no matter when you took the antibiotics
👉 Seed DS-01 Daily Synbiotic — the probiotic foundation
👉 Zenwise Digestive Enzymes — reduce bloating while you rebuild
👉 Psyllium Husk Capsules — prebiotic fiber and bowel normalization
👉 Multi Collagen Peptides — gut lining structural support
More from TummyCure:
- How Long Does Your Gut Take to Recover After Antibiotics?
- The Best Probiotic to Take After Antibiotics
- Your Gut Recovery Grocery List
- How to Restore Gut Bacteria After Antibiotics
- How Antibiotics Can Wreck Your Gut for a Year
- Can Leaky Gut Cause Anxiety and Depression?
- 7 Signs Your Gut Health Is Affecting Your Skin
- Seed DS-01 — Full Review
- The Complete Gut Health Guide
- 8 Signs Your Gut Desperately Needs a Probiotic
About the Author
Rachel Donnelly is a certified nutritional health coach and gut health writer who spent years struggling with IBS and bloating before making digestive wellness her specialty. She writes for TummyCure with one goal: cut through the noise and tell you what actually works. When she’s not deep in microbiome research, she’s fermenting things in her kitchen and losing arguments with her husband about whether kombucha counts as a dessert.
As an Amazon Associate we earn from qualifying purchases through some links in our articles.