Antibiotics disrupt your gut microbiome significantly — and recovery takes longer than most people realize. Here’s the complete timeline and the protocol that actually accelerates healing.
Antibiotics Saved You — Now Your Gut Needs Saving
Antibiotics are one of the most important medical developments in human history. They save lives, clear infections, and do exactly what they’re prescribed to do. But they do it indiscriminately — killing the harmful bacteria causing your infection and the beneficial bacteria in your gut that you need for digestion, immune function, mental health, and overall wellbeing.
A single course of antibiotics can reduce gut bacterial diversity by 25 to 50%. Some species recover quickly. Others take months. A few may not fully recover without deliberate intervention. The bloating, diarrhea, constipation, food sensitivities, fatigue, brain fog, and general feeling of being “off” that many people experience after antibiotics aren’t coincidental — they’re the downstream consequences of a gut microbiome that’s been significantly disrupted and is struggling to rebuild.
The good news: your gut microbiome is resilient. With the right support it can recover fully. The key phrase is “with the right support” — because the research is clear that passive recovery is slower and less complete than active, deliberate gut restoration.
Here’s everything you need to know about what happens to your gut after antibiotics, how long recovery takes, and what actually accelerates it.
What Antibiotics Actually Do to Your Gut Microbiome
Understanding the damage helps you understand what recovery requires. Antibiotics don’t selectively target the bacteria causing your infection — they target bacteria broadly, based on mechanism of action rather than species selection. Broad-spectrum antibiotics — amoxicillin, azithromycin, ciprofloxacin, clindamycin — are particularly impactful on the gut microbiome because they kill a wide range of bacterial species simultaneously.
The immediate effects are dramatic and measurable. Within 24 to 48 hours of starting a course of antibiotics, gut bacterial populations begin declining significantly. By the end of a standard 7 to 14 day course, the microbiome has typically lost substantial diversity — fewer different species, dramatically reduced populations of key beneficial strains like Lactobacillus and Bifidobacterium, and in some cases overgrowth of resistant harmful species that thrive in the ecological space left by the antibiotic’s destruction of their competitors.
Clostridioides difficile — C. diff — is the most serious consequence of this ecological disruption. C. diff is normally kept in check by the diverse bacterial community of a healthy gut. When antibiotics clear that community, C. diff can proliferate to dangerous levels, producing the severe diarrhea and colitis that requires its own antibiotic treatment. C. diff colitis affects approximately 1 in 30 people who take antibiotics — it’s the reason antibiotic stewardship and gut support after antibiotics matters clinically, not just for general wellness.
The Recovery Timeline — What the Research Shows
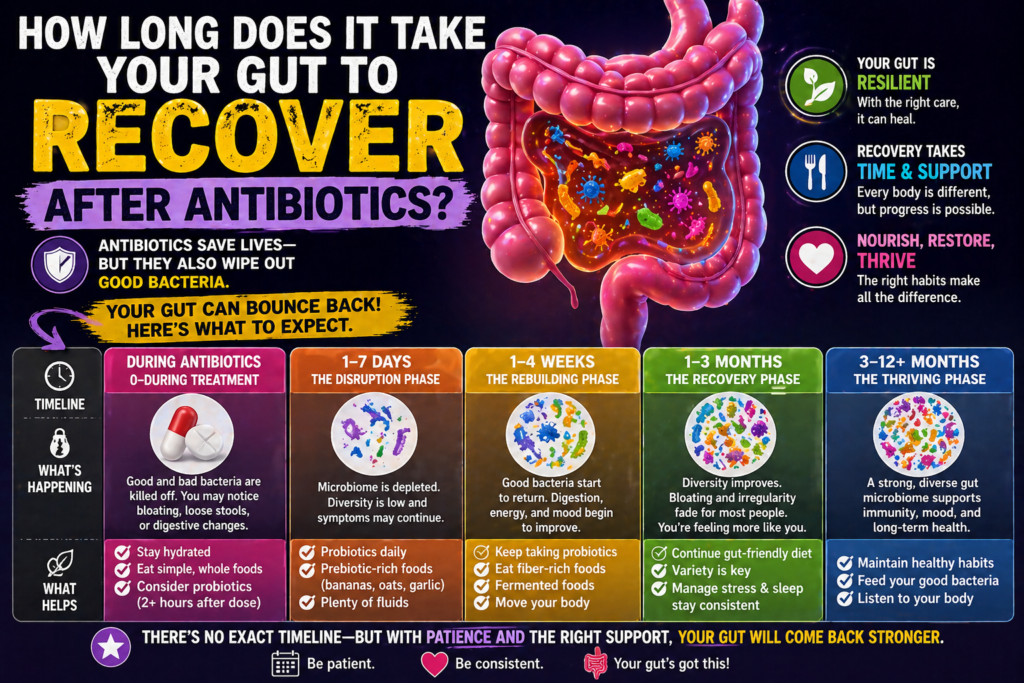
This is the question everyone wants answered — and the honest answer is more complex than most people expect. Recovery isn’t a single event. Different bacterial populations recover at different rates, and “recovery” means different things at different levels of analysis.
Week 1–2 After Finishing Antibiotics
The first week after completing a course of antibiotics is when symptoms are often at their worst — the antibiotic is still clearing your system, the microbiome disruption is at or near its peak, and your gut is in the process of trying to rebuild from a dramatically reduced bacterial population.
Common experiences during this period include loose stools or diarrhea, bloating, increased gas, fatigue, and food sensitivities to things that were previously tolerated fine. These are direct consequences of reduced beneficial bacterial populations and altered fermentation patterns in the gut.
The gut lining may also be more vulnerable during this period — beneficial bacteria that maintain tight junction integrity and produce butyrate for colonocyte health are depleted, temporarily increasing gut permeability. This is why post-antibiotic food sensitivities are so common — things that were previously contained by a robust gut barrier are now creating mild systemic immune responses.
Weeks 2–6: Early Rebuilding
For most people, the most obvious symptoms begin improving in the two to six week window after finishing antibiotics. The fastest-recovering bacterial species — primarily Lactobacillus strains — repopulate relatively quickly. Stool consistency begins normalizing. The most acute digestive symptoms ease.
However — and this is the part that surprises most people — feeling better doesn’t mean recovery is complete. The symptom improvement in weeks two to six reflects the recovery of the fastest-recovering species. The slower-recovering species — particularly Bifidobacterium, which are critical for immune function, gut lining health, and motility — are still well below their pre-antibiotic levels.
Research consistently shows that gut microbiome diversity — the number of different species present — remains measurably below baseline at the six-week mark after a standard antibiotic course. People who feel fine subjectively at six weeks have not necessarily achieved full microbiome recovery.
Months 2–6: Deeper Recovery
The six-month window is where the research picture gets interesting — and where passive versus active recovery diverges most significantly.
Studies tracking gut microbiome composition after antibiotic courses consistently show that without active intervention, microbiome diversity at the six-month mark is still measurably below pre-antibiotic baseline in a significant proportion of subjects. Some species that were present before the antibiotic course are still absent or at dramatically reduced levels six months later.
The studies that show more complete recovery at six months are those where subjects actively supported their microbiome through dietary intervention and probiotic supplementation. This is the research basis for the strong recommendation to actively support gut recovery rather than waiting for passive restoration.
Beyond 6 Months: The Chronic Disruption Risk
For some people — particularly those who took multiple antibiotic courses, took particularly broad-spectrum agents, or started with a less diverse baseline microbiome — antibiotic-induced gut disruption can persist for a year or longer without deliberate intervention. Some research suggests certain species may be permanently displaced after antibiotic exposure in some individuals — the ecological niche they occupied is taken over by other organisms that don’t vacate easily.
This chronic post-antibiotic disruption is increasingly recognized as a contributing factor in the development of IBS following antibiotic use — a well-documented phenomenon called post-infectious IBS. If you’ve noticed your gut has never quite been the same after a course of antibiotics years ago, this research may explain why. How antibiotics can disrupt your gut for a year or more covers the long-term impact in more detail.
Factors That Affect How Quickly Your Gut Recovers
Recovery timeline isn’t the same for everyone. These factors significantly influence how quickly — and how completely — your microbiome rebuilds after antibiotic exposure.
Which antibiotic you took. Broad-spectrum antibiotics like ciprofloxacin, clindamycin, and metronidazole produce more extensive microbiome disruption than narrow-spectrum agents. Clindamycin in particular is associated with particularly slow microbiome recovery and highest C. diff risk. The antibiotic type is the most significant determinant of disruption severity.
How long the course was. A 3-day course of amoxicillin produces less microbiome disruption than a 14-day course of the same antibiotic. Duration matters alongside drug type.
How many courses you’ve taken recently. Multiple antibiotic courses in a short period — particularly within the same year — produce cumulative microbiome disruption that takes significantly longer to recover from than a single isolated course.
Your baseline microbiome diversity. People with high baseline microbiome diversity before antibiotics recover faster and more completely than those who started with lower diversity. A diverse microbiome has more redundancy — when some species are depleted, others can partially compensate. A low-diversity microbiome has less buffer.
Your diet during and after antibiotics. A diet high in fiber and fermented foods during and after antibiotic treatment actively supports faster microbiome recovery. A diet high in processed food and sugar impedes it by feeding the wrong bacterial populations.
Whether you actively supplemented. This is the most modifiable factor. People who take a quality probiotic during and after antibiotics consistently show faster and more complete microbiome recovery in research studies compared to those who don’t.
The Active Recovery Protocol — What Actually Accelerates Healing
Start a Quality Synbiotic — Ideally During the Antibiotic Course
The most common question about probiotics and antibiotics is whether to take them during the course or only after. The research is clear: starting probiotics during the antibiotic course — not waiting until it’s finished — produces significantly better outcomes. Space the probiotic at least two hours away from each antibiotic dose to prevent the antibiotic from killing the probiotic bacteria before they can establish.
The probiotic doesn’t fully prevent antibiotic disruption — nothing does — but it reduces the severity of the disruption and provides a bacterial foundation that accelerates recovery once the course is complete.
After finishing the antibiotic, continue the probiotic daily for a minimum of 60 to 90 days. This is the window where the research shows the most significant difference between active and passive recovery. Don’t stop after two weeks because you feel better — the microbiome recovery that matters most is happening in the deeper bacterial populations that take longer to normalize.
Our top recommendation is Seed DS-01 Daily Synbiotic — 24 clinically studied strains including multiple Bifidobacterium species that are critical for post-antibiotic recovery, in an acid-resistant nested capsule with prebiotic included. The prebiotic component is particularly valuable post-antibiotics — you’re not just introducing bacteria, you’re providing the food they need to establish and multiply. 👉 Check the current price on Amazon.
We reviewed it in detail here: Seed DS-01 Review — Is It Actually Worth $50 a Month?
Load Up on Fermented Foods
Fermented foods introduce natural probiotic bacteria alongside the supplement bacteria — providing additional microbial diversity that supplements alone don’t fully replicate. Yogurt with live cultures, kefir, sauerkraut, kimchi, miso, and kombucha are all valuable during post-antibiotic recovery.
A landmark Stanford study published in Cell found that a high-fermented food diet produced greater microbiome diversity gains than a high-fiber diet alone — suggesting fermented foods deserve particular emphasis during recovery periods. Aim for at least one or two servings of fermented food daily throughout your recovery window. The fermented foods that make the biggest difference for gut health gives you the full list.
Prioritize Prebiotic Fiber
The bacteria you’re reintroducing — through both supplementation and fermented foods — need food to survive and multiply. Prebiotic fiber is that food. Without adequate prebiotic substrate, introduced bacteria pass through rather than colonizing.
The most important prebiotic foods for post-antibiotic recovery are: garlic, onions, leeks, asparagus, bananas (slightly underripe), oats, and Jerusalem artichokes. Diverse prebiotic sources feed a more diverse range of bacterial species — aim for variety rather than high doses of any single source.
Psyllium husk provides consistent soluble prebiotic fiber in a format that also helps normalize stool consistency during the post-antibiotic period when bowel habits are often disrupted. Psyllium husk capsules taken daily provide both prebiotic support and stool normalization simultaneously.
Support Your Gut Lining With Collagen
The post-antibiotic gut lining is more vulnerable than normal — depleted beneficial bacteria means less butyrate production, less tight junction maintenance, and temporarily increased intestinal permeability. Structural support for gut lining repair accelerates the return to normal barrier function.
Multi collagen peptides provide the structural proteins — particularly types I, III, and IV collagen — that the gut lining uses to maintain and repair tight junction integrity. Adding collagen peptides to your morning drink during the post-antibiotic recovery window supports the gut barrier rebuilding that beneficial bacteria restoration depends on.
Reduce Inflammation With Curcumin
Antibiotic-induced gut disruption produces a period of elevated gut inflammation as the immune system responds to the altered bacterial environment. Turmeric curcumin with black pepper reduces the NF-κB mediated gut inflammation that impedes recovery — creating a less inflammatory gut environment in which beneficial bacteria can reestablish more effectively.
Avoid the Foods That Impede Recovery
During the post-antibiotic recovery window, certain dietary choices actively slow microbiome rebuilding and deserve deliberate reduction:
Ultra-processed food starves beneficial bacteria of fiber, feeds harmful species with sugar, and contains emulsifiers that damage the gut lining. During post-antibiotic recovery it actively works against the rebuilding process.
Excess sugar and alcohol feed Candida and harmful bacteria that proliferate in the ecological space left by antibiotic disruption. Many people experience candida overgrowth symptoms after antibiotics — sugar and alcohol make this significantly worse.
Another course of antibiotics if avoidable — discuss with your doctor whether the antibiotic is truly necessary for whatever infection you’re treating. In some cases antibiotics are prescribed for viral infections where they have no benefit but full gut disruption cost.
Managing Specific Post-Antibiotic Symptoms
Diarrhea is the most common acute symptom. Most post-antibiotic diarrhea resolves within 1 to 2 weeks of finishing the course. If diarrhea is severe, watery, or accompanied by significant cramping and fever — this needs medical evaluation to rule out C. diff. Morning diarrhea specifically often has the same mechanisms at work as post-antibiotic diarrhea.
Bloating and gas typically peak in the first two weeks post-antibiotics and gradually improve as the microbiome rebuilds. Digestive enzymes with meals reduce the fermentation substrate reaching bacteria during the period when the microbiome composition is most disrupted. Zenwise Digestive Enzymes provides comprehensive enzymatic support during this period. 👉 Check the price on Amazon.
Constipation — less common than diarrhea but reported by some people after certain antibiotic types. Magnesium glycinate in the evening provides gentle motility support. Magnesium Glycinate is the gentlest and most appropriate daily option for post-antibiotic constipation.
Food sensitivities that developed or worsened typically reflect increased gut permeability during the recovery period. These usually improve as the microbiome rebuilds and gut barrier function normalizes — collagen support alongside probiotic supplementation accelerates this specifically.
Fatigue and brain fog reflect both the direct effects of the infection being treated and the gut-brain axis consequences of microbiome disruption. How gut disruption affects brain function and mood explains the mechanism — and the gut recovery protocol that addresses microbiome health also directly addresses these systemic symptoms over 4 to 8 weeks.
The Complete Post-Antibiotic Recovery Stack
Here’s the daily protocol that addresses every dimension of post-antibiotic gut recovery simultaneously:
- Seed DS-01 — daily, from day one of your antibiotic course through at least 90 days after finishing. The foundational microbiome rebuilding tool. 👉 Amazon price here.
- Zenwise Digestive Enzymes — with every meal during the acute recovery period. Reduces fermentation disruption while the microbiome rebuilds. 👉 Amazon price here.
- Psyllium husk capsules — daily with water. Prebiotic fiber for rebuilding bacteria plus stool normalization.
- Multi collagen peptides — daily in morning drink. Gut lining structural support during vulnerability window.
- Turmeric curcumin with ginger — daily. Anti-inflammatory support for the post-antibiotic gut inflammation period.
- Fermented foods — daily. Natural bacterial diversity that supplements alone don’t replicate.
Frequently Asked Questions
How long does it take for gut bacteria to recover after antibiotics?
The most acute symptoms typically improve within 1 to 4 weeks of finishing the course. Measurable microbiome diversity recovery takes 1 to 6 months depending on the antibiotic type, course length, individual baseline, and whether active support is provided. Without active intervention, some bacterial species may remain depleted for a year or longer. With consistent probiotic and dietary support, full functional recovery is achievable for most people within 3 to 6 months.
Should I take a probiotic while on antibiotics?
Yes — start at the same time as the antibiotic, spaced at least two hours apart from each dose. Research consistently shows better outcomes — less diarrhea during the course, faster microbiome recovery after — in people who take probiotics alongside antibiotics versus those who wait until the course is finished.
What is the best probiotic after antibiotics?
A multi-strain synbiotic with Lactobacillus and Bifidobacterium strains, acid-resistant delivery, and a prebiotic component. Seed DS-01 is our top recommendation — 24 clinically studied strains with prebiotic included in an acid-resistant nested capsule design. Read our full Seed DS-01 review here.
Why does my stomach still hurt months after antibiotics?
Post-antibiotic gut disruption takes longer to fully resolve than most people expect. If gut symptoms persist months after a course, it suggests incomplete microbiome recovery — some beneficial species are still at depleted levels. Active intervention with a quality probiotic, fermented foods, and prebiotic fiber is the most effective approach to accelerating recovery at any point after the antibiotic course.
Can antibiotics cause IBS?
Yes — post-infectious IBS following antibiotic use is a documented phenomenon. Significant antibiotic-induced microbiome disruption can produce IBS-like symptoms that persist long after the antibiotic course ends. The gut health approach for IBS and the approach for post-antibiotic recovery are closely related — both center on microbiome rebalancing and gut lining support.
What foods help gut recovery after antibiotics?
Fermented foods top the list — yogurt, kefir, sauerkraut, kimchi, miso. High-fiber plant foods provide prebiotic substrate for rebuilding bacteria. Bone broth and collagen-rich foods support gut lining repair. Foods to reduce: sugar, alcohol, ultra-processed food, and anything containing emulsifiers.
How do I know if my gut has recovered after antibiotics?
Subjective signs include resolution of post-antibiotic diarrhea or constipation, reduction in bloating and gas, improved energy and mental clarity, and return of normal tolerance for foods that became problematic post-antibiotics. Objectively, microbiome testing can measure diversity recovery — though this is rarely necessary for most people.
Your Gut Rebuilt Itself Once — It Can Do It Again
The gut microbiome is one of the most resilient ecosystems in the human body. It has been disrupted and rebuilt throughout human evolutionary history — by illness, by seasonal food changes, by environmental shifts. Antibiotic disruption is significant but it is not permanent.
The difference between full recovery and chronic post-antibiotic gut dysfunction is almost always active versus passive recovery. The people who actively support their microbiome rebuilding — with a quality synbiotic, fermented foods, prebiotic fiber, and gut lining support — consistently show faster, more complete recovery than those who wait for things to normalize on their own.
Start the protocol. Give it 90 days of consistency. Your gut has everything it needs to rebuild — it just needs the right support to do it efficiently.
More from TummyCure:
- How to Restore Gut Bacteria After Antibiotics
- How Antibiotics Can Wreck Your Gut for a Year
- Antibiotics Kill Both Good and Bad Bacteria
- Seed DS-01 — Full Probiotic Review
- Best Probiotic for IBS
- 10 Fermented Foods That Changed My Digestion
- Multi Collagen Peptides — Full Review
- Can Leaky Gut Cause Anxiety and Depression?
- The Complete Gut Health Guide
- 8 Signs Your Gut Desperately Needs a Probiotic
About the Author
Rachel Donnelly is a certified nutritional health coach and gut health writer who spent years struggling with IBS and bloating before making digestive wellness her specialty. She writes for TummyCure with one goal: cut through the noise and tell you what actually works. When she’s not deep in microbiome research, she’s fermenting things in her kitchen and losing arguments with her husband about whether kombucha counts as a dessert.
As an Amazon Associate we earn from qualifying purchases through some links in our articles.