Stomach pain every morning before you even eat anything? Here are the 7 most common reasons — and what to do about each one.
You Haven’t Eaten a Thing Yet — So Why Does Your Stomach Already Hurt?
You wake up and before you’ve done anything — before coffee, before breakfast, before getting out of bed — your stomach is already complaining. It might be a dull ache. It might be cramping or nausea. It might feel hollow and gnawing. And then, 20 or 30 minutes after you eat something, it fades. You feel fine. The rest of the day is normal.
This specific pattern — stomach pain that’s present on waking but improves after eating — is surprisingly common and surprisingly under-discussed. Most people assume it’s just hunger. Sometimes it is. But when it happens consistently, every morning, the causes run deeper than an empty stomach.
Here’s what’s actually going on — and what actually helps.
If you want to skip ahead: the two supplements that make the biggest difference for morning gut pain are a quality synbiotic for bacterial rebalancing and a digestive enzyme for meal-by-meal support. Read our Seed DS-01 review — 👉 check the price on Amazon.
Why an Empty Stomach Creates Pain
Your stomach produces gastric acid continuously — not just when you eat, but around the clock. During the day, food buffers that acid. It gives the acid something to work on and neutralizes it before it can irritate the stomach lining.
At night and into the morning, after 7 or 8 hours without food, there’s nothing in your stomach to buffer that acid. It sits directly against the stomach lining. For most people this causes no problem — the stomach lining is designed to handle acid. But for people with any degree of gastric sensitivity, inflammation, or compromised stomach lining integrity, that fasting acid pool causes the gnawing, hollow morning pain that improves almost immediately when food arrives to buffer it.
This is why the pain specifically gets better after eating — food neutralizes and dilutes the acid, removing the irritant that was causing the discomfort. The improvement after eating is actually a useful diagnostic clue that acid is involved in the mechanism.
Cause 1: Gastritis — Inflammation of the Stomach Lining
Gastritis is inflammation of the stomach lining — and it’s one of the most common causes of the specific pattern of morning stomach pain that improves after eating. Inflamed stomach lining is more sensitive to gastric acid than healthy tissue, so the fasting period overnight creates the conditions for significant morning discomfort.
The two most common causes of gastritis are H. pylori infection and chronic NSAID use. H. pylori is a bacterial infection of the stomach lining that’s more prevalent than most people realize — estimates suggest over half the global population carries it, though most people never develop symptoms severe enough to be diagnosed. NSAIDs — ibuprofen, aspirin, naproxen — erode the protective mucus layer of the stomach lining with regular use, leaving it vulnerable to acid damage.
If your morning stomach pain is burning or gnawing in character, located in the upper center or left of your abdomen, and you use NSAIDs regularly or have ever been told you might have H. pylori — gastritis is worth investigating with your doctor. It’s diagnosed easily and treated effectively once identified.
Cause 2: Peptic Ulcers
A peptic ulcer is an open sore in the stomach lining or the first part of the small intestine (duodenum). Like gastritis, ulcers are most painful when the stomach is empty because gastric acid contacts the raw ulcer surface with nothing to buffer it. Eating temporarily relieves the pain because food buffers the acid.
Duodenal ulcers — in the upper small intestine — classically produce pain that’s specifically worse 2–3 hours after eating and overnight, then better when food arrives. Gastric ulcers — in the stomach itself — may be worse during or after eating. The distinction matters for diagnosis.
H. pylori infection is responsible for the majority of peptic ulcers. Chronic NSAID use is the second most common cause. If your morning pain is sharp, burning, and located in the upper abdomen — and especially if it’s accompanied by any nausea, bloating, or dark stools — this needs medical evaluation rather than self-treatment.
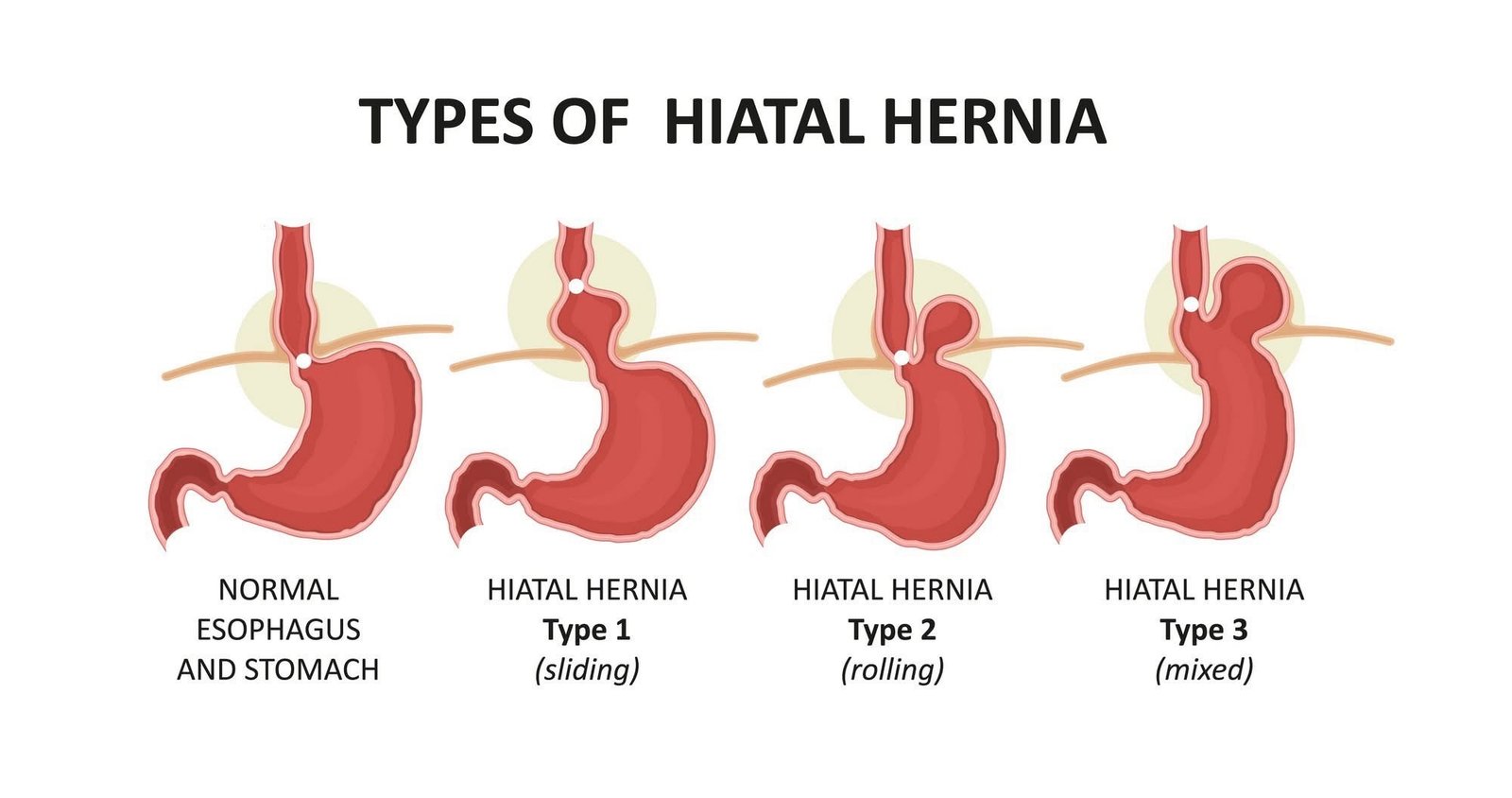
Cause 3: Acid Reflux and GERD
Gastroesophageal reflux disease — GERD — occurs when stomach acid regularly backs up into the esophagus. At night when you’re lying down, gravity no longer keeps acid in the stomach, and it’s more likely to reflux upward. By morning, the esophagus may be irritated from overnight acid exposure, producing that burning, uncomfortable morning feeling that improves when upright movement and food help clear and neutralize the acid.
GERD-related morning discomfort often has a burning quality and may be felt in the chest or throat as much as the stomach. Sour taste in the mouth on waking, hoarseness, and chronic throat clearing are other common morning signs of overnight acid reflux.
Understanding the real causes of acid reflux is important because the standard treatment — acid suppression — addresses the symptom without touching the underlying cause, and long-term use creates its own set of gut health problems.
Cause 4: IBS and Morning Gut Hypersensitivity
For people with IBS, the morning presents a unique combination of gut challenges. The natural overnight cortisol surge that accompanies waking stimulates gut motility. An overnight of fasting means the gut is empty and more sensitive. The gut-brain axis is at its most active in the transition from sleep to wakefulness.
All of these factors combine to make the morning the most symptomatic time of day for many IBS sufferers — producing cramping, nausea, or generalized abdominal discomfort that improves once the gut has been activated by food and the initial morning cortisol peak has passed.
The bacterial imbalance that underlies most IBS cases makes the gut hypersensitive to these normal morning stimuli. Rebalancing the microbiome with a quality synbiotic reduces that hypersensitivity over time. The right probiotic for your specific IBS type makes a meaningful difference — and understanding the realistic timeline for probiotic results keeps you consistent long enough for those results to develop.
Cause 5: Disrupted Gut Bacteria From the Night Before
What happened in your gut overnight directly shapes how your stomach feels when you wake up. If dinner was hard to digest — heavy, high-FODMAP, or eaten late — your gut bacteria have been fermenting that undigested material all night. By morning, the fermentation byproducts, gas, and organic acids produced overnight have been building for hours in your colon.
The result is a gut that wakes up already irritated, gassy, and uncomfortable before you’ve eaten anything. This is different from the acid-driven pain described above — it’s lower in the abdomen, more pressure-like or cramping rather than burning, and may be accompanied by bloating and an urgent need to use the bathroom before the pain fully resolves.
Taking a digestive enzyme with dinner is one of the most direct ways to address this cause — less undigested food at bedtime means less overnight fermentation and a less irritated gut in the morning. Zenwise Health Digestive Enzymes is our top recommendation for this purpose. 👉 Check the current price on Amazon.
Beyond the immediate dinner fix, rebalancing your gut bacteria with a probiotic reduces the amount of harmful fermentative activity that happens overnight regardless of what you ate. Signs your gut bacteria desperately need support are worth reviewing if this pattern is persistent.
Cause 6: Hunger and Low Blood Sugar
Sometimes the simplest explanation is the right one. After 8 hours without food, your blood sugar drops to its overnight low point right around the time you wake up. Low blood sugar produces physical symptoms that can easily be mistaken for stomach pain — nausea, shakiness, a hollow gnawing sensation, and general abdominal discomfort.
This type of morning discomfort resolves quickly after eating — usually within 15 minutes — because food rapidly raises blood sugar and removes the stimulus causing the discomfort. It tends to be worse if you ate dinner early, skipped dinner, or ate a very light dinner without much protein or fat to sustain blood sugar overnight.
If your morning stomach discomfort is accompanied by shakiness, lightheadedness, or difficulty concentrating until you eat — and resolves quickly and completely after breakfast — hunger and low blood sugar is the most likely explanation. Eating a more substantial dinner with adequate protein and healthy fat, or having a small protein-containing snack before bed, often resolves this pattern within a few days.
Cause 7: Anxiety and the Gut-Brain Morning Response
Anxiety has a remarkably direct effect on the gut. The gut-brain axis means that psychological stress and anxiety produce real, measurable physiological changes in digestive function — increased gut sensitivity, altered motility, changes in gut secretions. Morning is often the highest-anxiety period of the day for people who deal with anxiety — the transition from the relative calm of sleep to facing the day’s demands happens rapidly, and for some people the gut registers that transition as pain.
Morning anxiety-driven gut pain is often diffuse — hard to localize precisely — and accompanied by other anxiety symptoms like racing thoughts, tension, or a sense of dread. It tends to improve as the morning progresses and the anxiety settles, alongside or independently of eating.
This is another expression of the gut-brain connection that runs deeper than most people appreciate. Improving gut health genuinely reduces anxiety through its effects on serotonin production and vagal nerve communication — and managing anxiety genuinely reduces gut symptoms. The two are inseparable.
How to Tell What’s Causing Your Morning Stomach Pain
The character and location of your morning pain gives useful clues about the underlying cause.
Burning, gnawing pain in the upper abdomen that’s worse when the stomach is empty and better after eating — think gastritis, ulcer, or acid reflux. This needs medical evaluation if it’s persistent or severe.
Cramping or pressure in the lower or mid abdomen that may be accompanied by bloating or urgency — think IBS, overnight fermentation, or bacterial imbalance. This is the most common functional pattern and responds well to the enzyme and probiotic approach.
Diffuse, hard-to-locate discomfort accompanied by nausea, shakiness, or anxiety — think low blood sugar or anxiety-driven gut response. Responds to eating, time, and stress management.
Nausea without clear abdominal pain — can be acid reflux, low blood sugar, or gut bacterial issues. Rarely serious on its own but worth tracking.
What Actually Helps — The Protocol
Take a digestive enzyme with dinner every night. This is the most direct intervention for morning pain driven by overnight fermentation. Less undigested food reaching bacteria overnight means a less irritated, less gassy gut in the morning. Zenwise Digestive Enzymes — one capsule at the start of dinner. 👉 Check the price on Amazon.
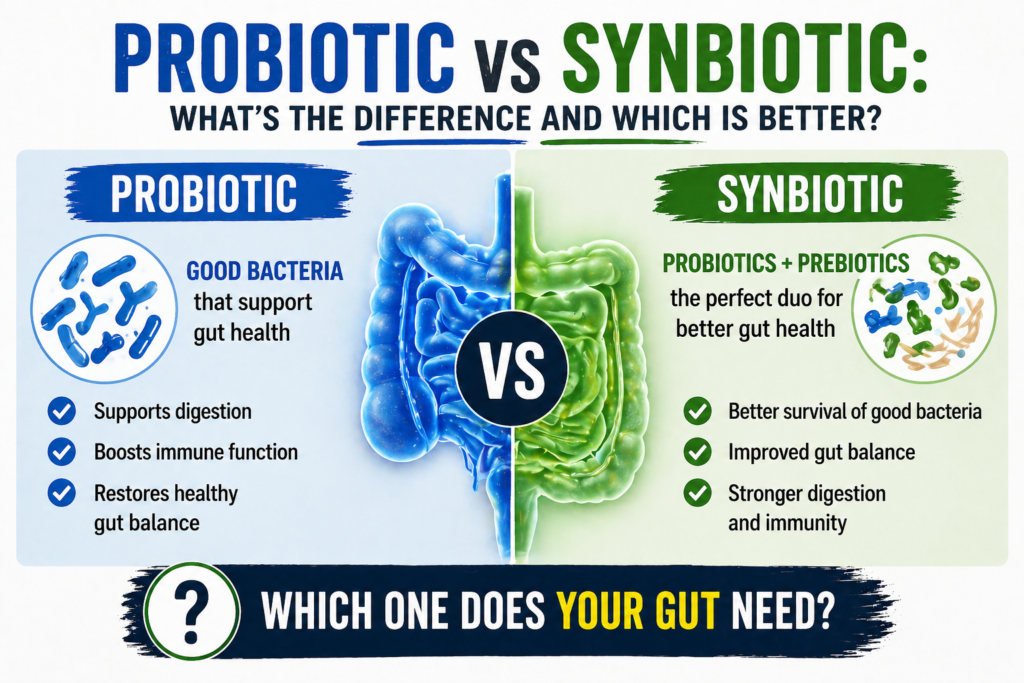
Start a quality synbiotic daily. Rebalancing your gut bacteria reduces the morning hypersensitivity that makes IBS and functional gut pain most pronounced. Seed DS-01 — 24 clinically studied strains, acid-resistant, prebiotic included. Take daily and give it 60–90 days. 👉 Check the price on Amazon.
Eat dinner earlier and lighter. Give your gut 2–3 hours to process dinner before sleep. Reduce high-FODMAP foods at dinner — garlic, onions, beans, large carb portions. The lighter and earlier your dinner, the less overnight fermentation and the calmer your morning gut.
Don’t skip breakfast — and eat it promptly. If low blood sugar or hunger is contributing, eating within 30 minutes of waking prevents the blood sugar drop that amplifies morning gut discomfort. A protein-containing breakfast is more effective than pure carbohydrates for sustaining blood sugar stability.
Try elevating the head of your bed slightly. For GERD-related morning pain, sleeping with your head elevated 6–8 inches reduces overnight acid reflux significantly. A wedge pillow is the easiest way to achieve this. Combined with not eating within 2–3 hours of bed, this makes a meaningful difference for acid-driven morning symptoms.
See your doctor if the pain is upper abdominal and burning. Gastritis, ulcers, and H. pylori need proper diagnosis and treatment. These are not conditions to manage indefinitely with self-treatment alone — they’re very treatable once identified.
Frequently Asked Questions
Why does my stomach hurt in the morning before I eat?
The most common reasons are gastric acid irritating an empty stomach lining, overnight fermentation from undigested dinner food, IBS-related morning gut hypersensitivity, or low blood sugar after overnight fasting. The character and location of the pain — burning vs cramping, upper vs lower abdomen — helps identify which cause is primary.
Why does eating make my morning stomach pain go away?
Food neutralizes and buffers gastric acid, removing the main irritant for acid-related morning pain. It also raises blood sugar if low, and activates the gut in a way that moves things through the system and relieves fermentation-related pressure. The improvement after eating is a useful clue that acid or hunger is involved.
Is morning stomach pain serious?
In most cases no — it’s functional and driven by the causes described above. However, upper abdominal burning pain that’s persistent, pain accompanied by blood in stool, unexplained weight loss, or progressive worsening warrants medical evaluation to rule out ulcers, gastritis, and other conditions that need specific treatment.
Can probiotics help with morning stomach pain?
Yes — for pain driven by gut bacterial imbalance, IBS hypersensitivity, or overnight fermentation. A quality probiotic reduces gut reactivity and fermentation activity over 4–8 weeks of consistent daily use. Our top recommendation is Seed DS-01.
What should I eat in the morning to help stomach pain?
For acid-related pain, bland, non-acidic foods that buffer stomach acid work best — oatmeal, toast, bananas, eggs. Avoid coffee on an empty stomach, citrus, and spicy foods first thing. For fermentation-related morning pain, eating promptly after waking helps move things through the system.
Can anxiety cause stomach pain in the morning?
Yes — and significantly. Morning is often the highest-anxiety period of the day and the gut-brain axis means that anxiety produces real, measurable gut symptoms including pain, nausea, and urgency. Managing the underlying anxiety alongside the gut health work produces the best outcomes.
Does coffee make morning stomach pain worse?
For most people with morning gut sensitivity, yes. Coffee is acidic, stimulates gastric acid secretion, and triggers gut motility — all of which worsen acid-related and IBS-related morning pain. Delaying coffee until after breakfast, or switching to a lower-acid option, often produces noticeable improvement.
Your Mornings Don’t Have to Start With Pain
Waking up uncomfortable every morning is one of those things that quietly lowers your quality of life in ways you stop noticing after a while. You just accept that mornings are rough and wait for your stomach to settle before your day actually starts.
It doesn’t have to be that way. The causes of morning stomach pain are specific and well understood — and for most people without an underlying structural issue, they respond well to targeted gut health support combined with smart dietary and lifestyle adjustments.
Start with what you can control tonight — a lighter, earlier dinner with a digestive enzyme. Add a daily synbiotic for the longer-term bacterial work. Give your gut the consistent support it needs and your mornings will look very different within a few weeks.
👉 Try Seed DS-01 on Amazon — our top pick for morning gut pain and IBS.
👉 Try Zenwise Digestive Enzymes on Amazon — take with dinner to reduce overnight fermentation.
More from TummyCure:
- Diarrhea Every Morning Then Fine — Here’s Why
- Why Does My Stomach Hurt After Eating But Goes Away After Pooping?
- Why Do I Bloat More at Night Than in the Morning?
- Seed DS-01 — Full Review
- Zenwise Digestive Enzymes — Full Review
- Best Probiotic for IBS
- Living With Acid Reflux
- Why Does Coffee Make My Stomach Hurt in the Morning?
- Is Your Gut Sabotaging Your Mental Health?
- The Complete Gut Health Guide
- Stomach Gurgling at Bedtime — Here’s Why
About the Author
Rachel Donnelly is a certified nutritional health coach and gut health writer who spent years struggling with IBS and bloating before making digestive wellness her specialty. She writes for TummyCure with one goal: cut through the noise and tell you what actually works. When she’s not deep in microbiome research, she’s fermenting things in her kitchen and losing arguments with her husband about whether kombucha counts as a dessert.
As an Amazon Associate we earn from qualifying purchases through some links in our articles.