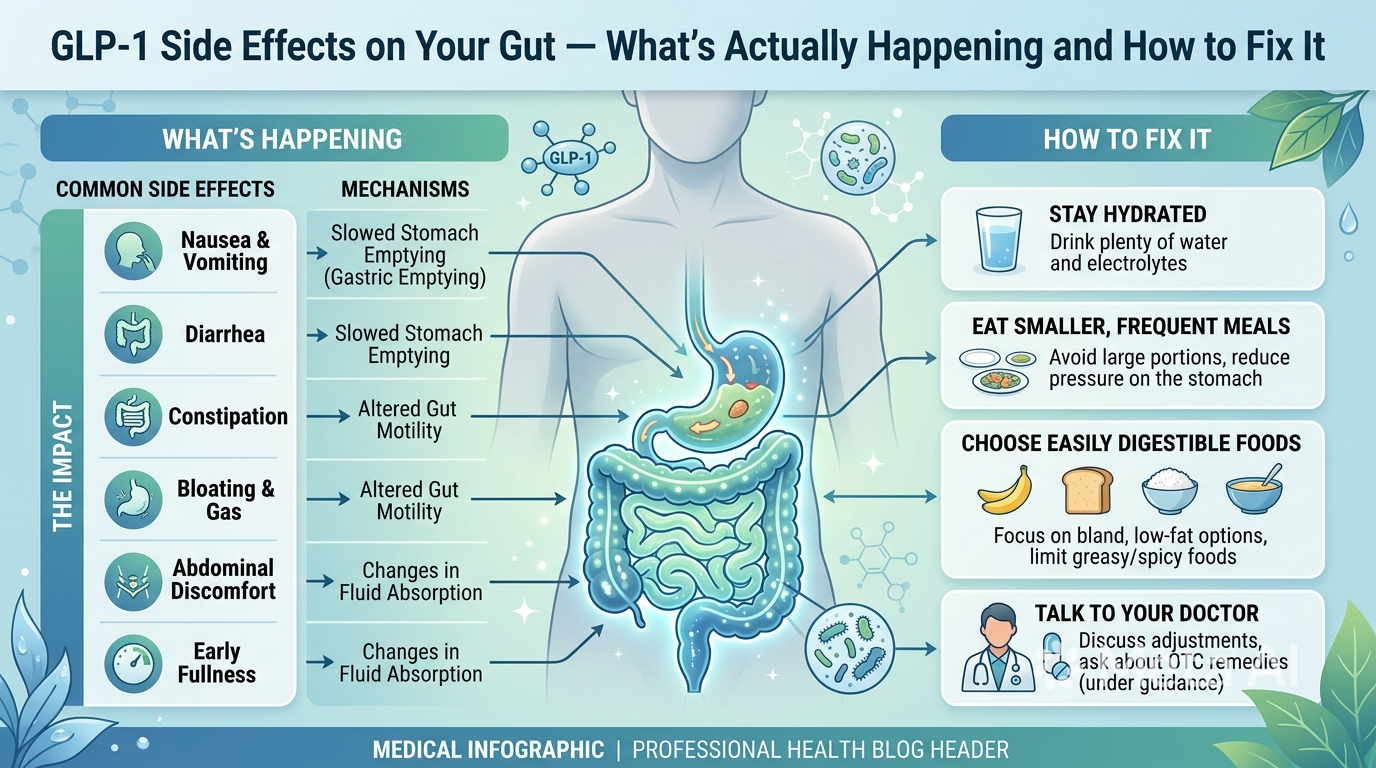
Constipation is one of the most common and persistent GLP-1 side effects. Here’s why it happens, why the standard advice often fails, and the complete protocol that actually works.
Nobody Warned You That Losing Weight Would Mean Not Being Able to Go
The appetite suppression is working. The scale is moving. You feel like you’re finally getting somewhere — and then you realize you haven’t had a proper bowel movement in four or five days. Your stomach feels full even when you haven’t eaten much. You’re bloated and uncomfortable in a way that has nothing to do with what you’ve eaten.
Constipation on Wegovy, Ozempic, Mounjaro, and other GLP-1 medications is one of the most common and most persistently underreported side effects of these drugs. Clinical trials put the incidence at anywhere from 20 to 40% — some real-world surveys suggest it’s even higher. And unlike nausea, which typically improves as your body adapts, constipation on GLP-1 medications tends to persist as long as you’re taking the drug at therapeutic doses.
Here’s why it happens and — more usefully — what actually works to manage it.
Why GLP-1 Medications Cause Constipation
Understanding the mechanism makes the solution much clearer. GLP-1 receptor activation slows your entire digestive tract — not just your stomach. The same mechanism that delays gastric emptying and makes you feel full longer also reduces colonic motility — the muscular contractions that move stool through your large intestine toward elimination.
When colonic motility slows, stool moves through your colon more slowly than it should. As stool sits in the colon longer, the colon continues absorbing water from it — it’s designed to do this. The longer stool sits, the more water gets absorbed, the harder and drier it becomes. Hard, dry stool is difficult and uncomfortable to pass. And if it sits long enough, the urge to go diminishes as the rectum adapts to the presence of stool — making the problem self-compounding.
Several factors specific to GLP-1 treatment make this worse:
Reduced food intake. Less food moving through the gut means less bulk stimulating colonic contractions. Your colon needs material to push — when you’re eating significantly less, there’s less natural motility stimulus.
Blunted thirst. GLP-1 medications suppress thirst alongside hunger. Most people on these medications are chronically underhydrated without realizing it — and dehydration directly worsens constipation by causing the colon to extract even more water from already-slow stool.
Reduced fiber intake. Eating less often means eating less fiber — and fiber is the primary substrate that stimulates and feeds the gut bacteria responsible for maintaining normal colonic motility.
This is a constipation driven by motility impairment — not by diet alone. Which is why simply telling someone to eat more fiber and drink more water often doesn’t fully solve GLP-1 constipation the way it might solve dietary constipation.
What Doesn’t Work — And Why
Before getting to what does work, it’s worth being direct about what often doesn’t.
Simply adding insoluble fiber — bran, wheat fiber — often makes things worse. Insoluble fiber adds bulk to stool. When the colon is barely contracting, more bulk just means more stool that doesn’t move. Adding volume to a system with impaired motility compounds the problem rather than solving it. This is why the bran flake approach that works for dietary constipation fails repeatedly for GLP-1 constipation.
Stimulant laxatives are a short-term fix with long-term downsides. Senna, bisacodyl, and similar stimulant laxatives work by irritating the colon wall to force contractions. They work in the short term but with regular use, the colon can become dependent on chemical stimulation to contract — making natural motility even worse over time. For occasional relief they’re fine. As a daily management strategy for ongoing GLP-1 constipation, they’re not the right approach.
Drinking more water alone isn’t sufficient. Hydration matters and you absolutely should be drinking more — but water alone can’t overcome the motility impairment that’s the primary driver of GLP-1 constipation. You need to address the motility piece directly alongside hydration.
What Actually Works
Magnesium Glycinate — The Most Effective Daily Intervention
Magnesium glycinate is the single most effective supplement for GLP-1 constipation — and it works through mechanisms directly relevant to what’s causing the problem.
Magnesium draws water into the intestines through osmosis — keeping stool soft and hydrated even when the colon is moving slowly. It also supports smooth muscle function throughout the gut — the same smooth muscles that GLP-1 medications are suppressing. While it can’t fully override a pharmacologically induced motility reduction, it meaningfully counteracts it by providing the mineral that gut smooth muscles require to contract efficiently.
Magnesium glycinate specifically — the chelated form — is the right choice here. Magnesium oxide causes urgency and cramping. Magnesium citrate is better but still on the dramatic side. Magnesium glycinate is gentle, well-absorbed, and produces consistent daily relief without the unpredictable urgency that makes other forms problematic when you’re already dealing with an unpredictable gut.
Take it in the evening — 500mg before bed. Most people notice meaningfully more regular, easier morning bowel movements within a week. Read the full breakdown here: Magnesium Glycinate — The Sleep and Gut Supplement That Actually Delivers.
Psyllium Husk — Soluble Fiber That Normalizes Rather Than Bulks
Psyllium husk is the fiber supplement that actually works for GLP-1 constipation — and the reason it works where insoluble fiber fails is the type of fiber it provides.
Psyllium is almost entirely soluble fiber. It absorbs water and forms a gel — which lubricates the intestinal wall, keeps stool hydrated and soft regardless of how slowly it’s moving, and has been clinically shown to normalize transit time in both constipation and diarrhea. The gel-forming property means it helps stool stay soft through extended time in a slow-moving colon in a way that insoluble fiber simply can’t.
The clinical evidence for psyllium specifically for constipation is among the strongest of any fiber supplement — multiple randomized controlled trials showing significant improvements in stool frequency and consistency. And the capsule format eliminates the texture problem that makes powder-form psyllium so unpleasant.
Two capsules daily with a large glass of water — non-negotiable with psyllium. The fiber needs water to do its job. Full review here: Psyllium Husk Capsules — The Most Research-Backed Fiber Supplement You’re Probably Not Taking.
A Quality Probiotic — For the Bacterial Motility Component
Your gut bacteria directly regulate colonic motility — Bifidobacterium strains in particular produce compounds that stimulate intestinal contractions and maintain normal transit time. When the microbiome is disrupted by altered transit from GLP-1 medications, the bacterial support for normal motility decreases.
Specific probiotic strains — particularly Bifidobacterium lactis and Bifidobacterium longum — have clinical evidence for improving bowel frequency and reducing constipation. A multi-strain synbiotic that includes these strains addresses the bacterial motility component that supplements alone can’t fully cover.
Seed DS-01 includes multiple Bifidobacterium strains studied for exactly this purpose. Give it 4–8 weeks of consistent daily use to see its full motility benefit. 👉 Check the current price on Amazon.
Intentional Hydration — On a Schedule
You cannot rely on thirst on GLP-1 medications. The medications suppress thirst signals alongside hunger — meaning your body’s normal hydration cues are unreliable. Set water reminders and drink on a schedule regardless of whether you feel thirsty.
Aim for a minimum of 8–10 glasses of water spread throughout the day. Drink between meals rather than with them — drinking large amounts with meals can worsen nausea and slow already-slow gastric emptying further. Herbal teas count toward your fluid total. Caffeinated drinks are a net negative for hydration — they have a mild diuretic effect that partially offsets the fluid they provide.
Movement — More Than You Think You Need
Physical movement directly stimulates colonic motility through both mechanical and neurological mechanisms. Walking specifically — the up-down movement and core engagement of walking — is one of the most reliable natural stimulants of gut motility available. Even 20 to 30 minutes of walking daily produces measurable improvement in colonic transit time.
On GLP-1 medications where you’re eating less, having less energy initially, and dealing with nausea that makes movement feel unappealing — this is exactly when movement matters most for gut function. A post-meal walk is particularly effective — the gastrocolic reflex from eating combined with the movement stimulus creates the strongest natural motility response of the day.
Toilet Posture — The Squatty Potty Effect Is Real
The standard Western toilet sitting position creates a suboptimal anorectal angle for defecation — the puborectalis muscle remains partially contracted, creating a kink in the lower rectum that makes complete emptying harder. Elevating your feet on a stool while sitting on the toilet — creating a more squatting-like position — straightens this angle and makes passing stool significantly easier, requiring less straining.
This is particularly relevant for GLP-1 constipation because hard, slow-moving stool is already more difficult to pass — any mechanical assistance matters. A simple footstool under your feet while on the toilet is one of the most effective and most underutilized tools for difficult-to-pass stool.
The Combination Protocol That Works Best
These interventions work best together rather than individually. The full daily protocol for GLP-1 constipation:
- Morning: Psyllium husk capsules with a large glass of water. Seed DS-01 probiotic with breakfast.
- Throughout the day: Water on schedule — minimum 8 glasses regardless of thirst. Post-meal walks especially after your largest meal.
- Evening: Magnesium glycinate 500mg before bed. Light, low-fat dinner eaten early enough to allow some digestion before sleep.
- Every meal: Digestive enzymes — Zenwise Digestive Enzymes to reduce the bloating and gas that compound constipation discomfort. 👉 Check the price on Amazon.
Most people following this protocol consistently notice meaningful improvement within 5 to 7 days. Full resolution of GLP-1 constipation is the goal but may require ongoing management — this is a side effect that tends to persist with the medication rather than fully resolving through adaptation.
When to Contact Your Prescriber
Most GLP-1 constipation is uncomfortable but manageable. Contact your prescriber if:
- You haven’t had a bowel movement in more than a week despite management strategies
- Constipation is accompanied by significant abdominal pain or bloating that is worsening
- You have nausea or vomiting alongside constipation — this combination can suggest more significant GI motility issues
- You notice blood in your stool
- Constipation is severe enough that you’re straining significantly — prolonged straining can cause hemorrhoids and other anorectal problems
Dose reduction is a legitimate option if constipation is significantly affecting your quality of life — discuss with your prescriber whether a lower dose with slower titration might provide the weight loss benefits with more manageable gut effects.
Frequently Asked Questions
Why does Wegovy cause constipation?
GLP-1 receptor activation slows colonic motility — the muscular contractions that move stool through your large intestine. Combined with reduced food intake and blunted thirst from the medication, stool moves more slowly, absorbs more water, becomes harder, and is more difficult to pass.
Does Ozempic constipation go away?
Unlike nausea which typically improves with adaptation, constipation on GLP-1 medications tends to persist because it’s driven by ongoing motility reduction rather than an adaptation response. Most people need ongoing management strategies for constipation throughout their time on the medication.
What is the best laxative for Ozempic constipation?
We’d steer away from stimulant laxatives as a daily solution — they address the symptom without the cause and can create dependency. Magnesium glycinate and psyllium husk together address the motility and stool consistency components in a sustainable daily way. For occasional acute relief, osmotic laxatives like MiraLax are preferable to stimulant types.
Can I take magnesium for constipation on semaglutide?
Yes — magnesium glycinate specifically is one of the most appropriate and well-tolerated daily interventions for GLP-1 constipation. It supports smooth muscle function and draws water into the intestine gently and consistently. Take 500mg in the evening.
How much water should I drink on Wegovy for constipation?
Aim for at least 8–10 glasses daily on a schedule — don’t rely on thirst signals which GLP-1 medications suppress. Spread water intake throughout the day rather than in large amounts at once, and prioritize drinking between meals rather than with them.
You Don’t Have to Choose Between the Weight Loss and Gut Comfort
GLP-1 medications are producing results for millions of people that decades of dieting couldn’t achieve. The constipation side effect is real and frustrating — but it’s manageable with the right consistent approach. The magnesium, psyllium, probiotic, hydration, and movement combination addresses the problem from multiple angles simultaneously and for most people produces a meaningful improvement that makes the medication tolerable long-term.
Don’t stop a medication that’s working because of a side effect that can be managed. Give the protocol above a solid two weeks and see what changes.
More from TummyCure:
- Complete GLP-1 Gut Side Effects Guide
- Magnesium Glycinate — Full Review
- Psyllium Husk Capsules — Full Review
- Seed DS-01 — Full Probiotic Review
- Zenwise Digestive Enzymes — Full Review
- Why Am I Always Constipated?
- Why Does Ozempic Make Your Stomach Hurt?
- Why Do I Bloat More at Night?
- The Complete Gut Health Guide
About the Author
Rachel Donnelly is a certified nutritional health coach and gut health writer who spent years struggling with IBS and bloating before making digestive wellness her specialty. She writes for TummyCure with one goal: cut through the noise and tell you what actually works. When she’s not deep in microbiome research, she’s fermenting things in her kitchen and losing arguments with her husband about whether kombucha counts as a dessert.
As an Amazon Associate we earn from qualifying purchases through some links in our articles.