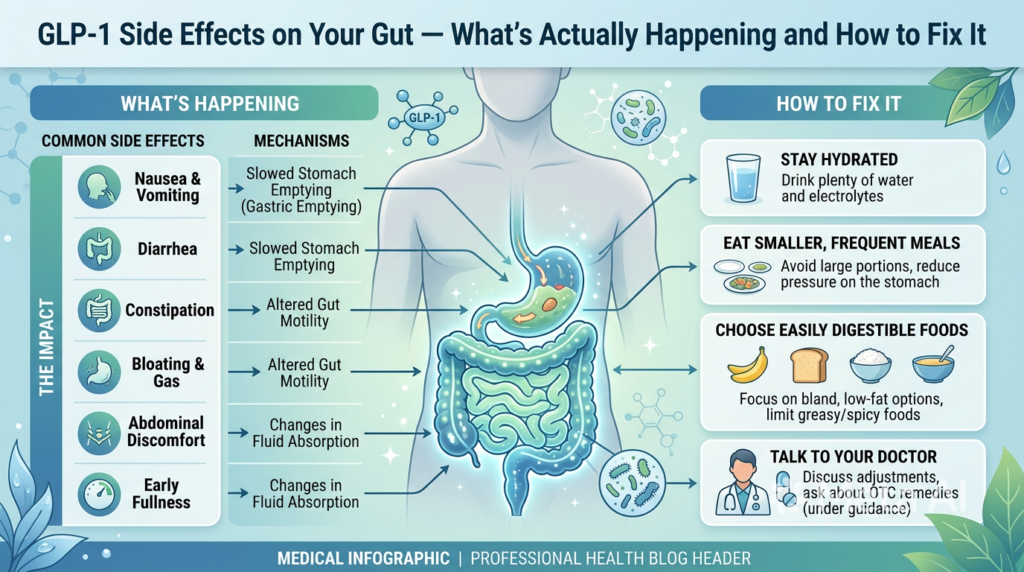
Nausea, constipation, bloating, gastroparesis — GLP-1 medications like Ozempic and Wegovy do a number on your gut. Here’s why it happens and the complete protocol that actually helps.
GLP-1 Medications Are Changing Lives — But Nobody Warned You About What They’d Do to Your Gut
Semaglutide. Tirzepatide. Ozempic. Wegovy. Mounjaro. If you’re taking one of these medications — or thinking about it — you already know about the weight loss results. What most people aren’t fully prepared for is what these drugs do to your digestive system while they’re doing their job.
GLP-1 receptor agonists work precisely because they slow your digestive system down. That’s not a bug — it’s the mechanism. Slower gastric emptying, reduced appetite, blunted gut motility. These are the features that produce weight loss. And they’re also exactly why a significant proportion of people on GLP-1 medications deal with nausea, vomiting, constipation, diarrhea, acid reflux, and gut pain that ranges from inconvenient to genuinely debilitating.
This guide covers everything — why GLP-1 medications affect your gut the way they do, which side effects are most common, how long they typically last, and — most importantly — what actually helps manage them so you can stay on the medication long enough to get the results you’re after.
How GLP-1 Medications Work — And Why Your Gut Pays the Price
GLP-1 stands for glucagon-like peptide-1 — a hormone naturally produced in your small intestine after eating. In normal physiology, GLP-1 signals your pancreas to release insulin, tells your brain you’re full, and slows gastric emptying to extend the feeling of satiety. GLP-1 receptor agonist medications mimic this hormone at much higher and more sustained concentrations than the body naturally produces.
The result is a digestive system running in a state of constant, pharmacologically induced slowdown. Your stomach empties more slowly. Your gut motility decreases. The signals telling your brain you’re full are constantly amplified. Appetite drops dramatically. Food intake decreases. Weight loss follows.
But your gut is an ecosystem — not just a pipe. When you significantly slow its function, alter its motility patterns, and change how food moves through it, the entire system feels the effects. The bacteria in your microbiome respond to altered transit times. Digestive enzyme secretion changes. The vagus nerve signaling that regulates all of this gets disrupted. And the symptoms that result are the downstream consequences of a digestive system whose normal operating parameters have been fundamentally altered.
Understanding this isn’t just academic. It tells you why certain interventions help and others don’t — because you’re not treating random side effects. You’re managing the consequences of specific, predictable physiological changes.
The Most Common Gut Side Effects — What’s Really Happening
Nausea — The Most Reported Side Effect
Nausea affects up to 40–50% of people starting GLP-1 medications — it’s by far the most commonly reported side effect and the most common reason people discontinue. It typically peaks in the first 4–8 weeks of treatment and improves as your body adapts to the medication, but for some people it persists at lower intensity throughout treatment.
The mechanism is twofold. GLP-1 receptors are present in the brainstem area that controls nausea and vomiting — direct receptor activation in this area produces nausea independently of what’s happening in your stomach. And slowed gastric emptying means food sits in your stomach longer than usual, producing the uncomfortable fullness and nausea that delayed emptying always causes.
What makes GLP-1 nausea worse: eating too much in one sitting, eating fatty or rich foods, eating too quickly, eating too close to your injection or dose, and lying down after eating. Each of these compounds the already-slowed gastric emptying in ways that dramatically increase nausea intensity.
What actually helps: small frequent meals rather than large ones, avoiding high-fat foods during peak nausea periods, eating slowly and stopping well before fullness, staying upright for at least two hours after eating, and ginger — which has genuine antiemetic properties through its effect on gut serotonin receptors. The ginger component in turmeric curcumin gummies with ginger provides this in a convenient daily form alongside the anti-inflammatory benefits.
For most people nausea is worst in the first 2–4 weeks after a dose increase and becomes manageable with the dietary adjustments above. The dose escalation schedules used with GLP-1 medications are specifically designed to minimize nausea — if your prescriber is increasing your dose and nausea is severe, going more slowly on the titration is a legitimate clinical option worth discussing.
Constipation — The Underreported Problem
Constipation is actually more prevalent on GLP-1 medications than nausea in some studies — it just gets less attention because people are less likely to report it or because nausea is more immediately distressing. Estimates suggest 20–40% of GLP-1 users experience significant constipation, particularly as doses increase.
The mechanism is straightforward. GLP-1 receptor activation directly slows colonic motility — the contractions that move stool through your large intestine. Combined with reduced food intake (less material moving through the gut) and often reduced fluid intake (thirst is also blunted), the result is stool that moves too slowly, absorbs too much water, becomes hard, and is difficult to pass.
GLP-1 constipation is a motility problem — not a fiber or hydration problem in the traditional sense. Adding more fiber to a gut that’s barely contracting can actually make things worse by adding more bulk that sits and doesn’t move. The solution needs to address motility alongside stool consistency.
Magnesium glycinate is one of the most effective interventions here — it works by drawing water into the intestines and supporting smooth muscle function, addressing both the stool consistency and the motility component. Magnesium glycinate specifically — not magnesium oxide — provides gentle consistent relief without urgency. Take it in the evening and most people notice meaningful improvement within a week.
Psyllium husk provides soluble fiber that softens stool and normalizes transit without the bulk-loading problem of insoluble fiber. Psyllium husk capsules taken daily with a full glass of water are one of the most evidence-backed approaches for this type of constipation.
Staying intentionally hydrated is essential — thirst suppression from GLP-1 medications means many people are chronically dehydrated without realizing it, which compounds constipation significantly. Set water reminders if necessary rather than relying on thirst signals that the medication has blunted.
The comprehensive picture of why constipation persists despite doing everything right applies directly to GLP-1 users — and the solutions there map exactly to what works on these medications.
Diarrhea — Less Common But Significant
Diarrhea on GLP-1 medications is less common than constipation overall but affects a meaningful minority of users — particularly in the early weeks and after dose increases. For some people the pattern alternates — constipation at some points and diarrhea at others as the gut adjusts to altered motility patterns.
GLP-1-related diarrhea typically results from altered intestinal transit — the gut, trying to compensate for slowed gastric emptying, occasionally overcorrects with increased colonic motility. High-fat meals are a particular trigger because fat is the macronutrient most affected by altered GLP-1-driven digestion — incompletely processed fat in the colon stimulates urgent contractions and loose stools.
Digestive enzymes — particularly lipase — help by ensuring fat is properly broken down before it reaches the colon. Zenwise Digestive Enzymes taken at the start of every meal provides the lipase and broader enzymatic support needed to compensate for the altered digestion GLP-1 medications produce. 👉 Check the current price on Amazon.
Probiotic supplementation also helps stabilize the gut bacterial environment that GLP-1-altered transit disrupts. The morning diarrhea pattern that many GLP-1 users report has specific mechanisms that targeted probiotic support addresses over time.
Gastroparesis — When Gastric Emptying Gets Too Slow
This is the most serious gut side effect of GLP-1 medications and one that’s received significant attention in the medical literature. GLP-1 receptor agonists slow gastric emptying as part of their intended mechanism — but in some people this effect is exaggerated, producing symptoms consistent with gastroparesis: severe nausea, vomiting, early satiety so pronounced you can barely eat, feeling full hours after a small meal, and abdominal pain.
Gastroparesis-level symptoms on GLP-1 medications are particularly problematic for several reasons beyond the symptoms themselves. Severely delayed gastric emptying can affect the absorption of other medications you’re taking — including oral medications that are supposed to be absorbed in the small intestine but are sitting in a stomach that barely empties. This is clinically significant for people on blood pressure medications, thyroid medications, and other time-sensitive drugs.
If you’re experiencing severe nausea, vomiting, or inability to eat more than tiny amounts on GLP-1 medication — this needs medical evaluation rather than self-management. Your prescriber may need to reduce your dose, slow your titration schedule, or in some cases pause the medication temporarily.
For milder gastroparesis-adjacent symptoms — persistent early satiety, food sitting heavy for hours, moderate nausea — the dietary adjustments for nausea apply here too: very small frequent meals, liquid calories during the worst periods, low-fat food choices, and upright posture after eating. Why you feel full so fast covers the gastroparesis mechanism in detail alongside what helps.
Iberogast — the European herbal formula with 60 years of clinical evidence — has prokinetic properties that help improve gastric emptying rate. Iberogast’s motility-regulating properties make it one of the more useful non-pharmaceutical tools for GLP-1 related gastric slowdown.
Acid Reflux and GERD
Acid reflux is a commonly reported but often overlooked GLP-1 side effect. The mechanism involves several factors combining: slowed gastric emptying means more acid-containing stomach contents sitting longer, increasing the opportunity for reflux. GLP-1 receptor activation may reduce lower esophageal sphincter tone in some people. And the altered eating patterns — eating less but sometimes eating too much at once and too quickly — create reflux-prone conditions.
For people who already had acid reflux before starting GLP-1 medications, the medication often worsens it significantly. For people without pre-existing reflux, new-onset heartburn on these medications is not uncommon.
The management approach is the same as for GERD generally — small meals, avoiding eating close to bed, staying upright after meals, avoiding trigger foods — but with the added GLP-1 context that you also need to be very careful not to overeat in any single sitting, as even moderate meal sizes can overwhelm a significantly slowed stomach. Managing acid reflux long term covers the full picture of what actually helps beyond antacids.
Bloating and Gas
Bloating is extremely common on GLP-1 medications — driven by multiple converging factors. Slowed transit means gas produced by bacterial fermentation stays in the gut longer before being expelled. Altered eating patterns can include more FODMAP-heavy foods in small amounts that nonetheless accumulate. And the gut microbiome disruption that comes with significantly altered transit times shifts bacterial populations toward more gas-producing compositions over time.
The pattern of bloating that builds through the day is particularly common on GLP-1 medications — the cumulative gas accumulation from slowed transit is worst by evening. Digestive enzymes with every meal reduce fermentation substrate. A quality probiotic addresses the bacterial composition driving excess gas production. And eating earlier, lighter dinners gives the gut more time to process before sleep.
The Gut Microbiome on GLP-1 Medications — What the Research Is Showing
One of the most interesting emerging areas of GLP-1 research is what these medications do to the gut microbiome — and it’s more complex than most people realize.
Early research suggests that GLP-1 receptor agonists do produce measurable changes in gut microbiome composition — some potentially beneficial, some potentially problematic. The beneficial changes appear related to the reduced caloric intake and altered substrate availability for bacteria. The potentially problematic changes relate to significantly slowed transit times — bacteria normally kept in check by regular movement through the gut have more time to proliferate in a slower environment.
The practical implication is that active microbiome support during GLP-1 treatment is worthwhile — not just for managing side effects but for maintaining the gut bacterial health that underlies immune function, mental health, and long-term metabolic outcomes. Seed DS-01 is our top recommendation for comprehensive microbiome support during GLP-1 treatment. 👉 Check the current price on Amazon.
The Digestive Enzyme Deficit — Why GLP-1 Users Often Need Support
This is an underappreciated aspect of GLP-1 gut effects. Normal digestive enzyme secretion is partly triggered by food moving through the digestive system at normal speed — the hormonal and nerve signals that tell your pancreas to release enzymes are timed to normal gastric emptying. When gastric emptying is significantly slowed by GLP-1 medications, that timing is disrupted. Enzyme secretion becomes less well-coordinated with food arrival in the small intestine.
The result is that even on the smaller meals GLP-1 users eat, food may not be optimally broken down — contributing to the bloating, gas, and discomfort that many users experience. This is why digestive enzyme supplementation specifically helps many GLP-1 users beyond just the general gut health benefits.
Taking a comprehensive digestive enzyme at the start of every meal compensates for the disrupted enzyme timing that GLP-1 medications produce. Zenwise Health Digestive Enzymes covers the full spectrum — amylase, lipase, protease, lactase, bromelain, and papain — and many GLP-1 users notice reduced post-meal discomfort within the first week of consistent use. 👉 Check the current price on Amazon.
Nutritional Considerations During GLP-1 Treatment
The dramatic reduction in food intake that GLP-1 medications produce — which is the mechanism of the weight loss — creates nutritional considerations that are easy to overlook when you’re focused on the scale moving in the right direction.
Protein intake becomes critical. Rapid weight loss without adequate protein intake leads to significant muscle loss alongside fat loss — and muscle mass is metabolically critical for long-term weight maintenance. On GLP-1 medications, getting adequate protein on dramatically reduced caloric intake requires deliberately prioritizing protein at every meal. Aim for protein first — before vegetables, carbohydrates, or fats — to ensure you hit your target before satiety stops you eating.
Micronutrient deficiencies are a genuine risk. Eating significantly less food means consuming significantly fewer vitamins and minerals. B12, folate, iron, zinc, and vitamin D are the micronutrients most commonly deficient in people on very low caloric intake. A comprehensive multivitamin taken consistently is prudent during GLP-1 treatment — not optional.
Gut lining support matters more during rapid weight loss. Rapid weight loss produces metabolic and inflammatory changes that can affect gut lining integrity. Collagen peptide supplementation during this period supports the structural repair of the gut lining alongside the dietary upheaval of GLP-1 treatment. Multi collagen peptides added to whatever you’re eating or drinking is low effort and high value during this period.
Hydration requires active management. GLP-1 medications blunt thirst alongside hunger. Dehydration compounds every gut side effect — constipation, nausea, and bloating all worsen significantly when fluid intake is inadequate. Drink water on a schedule rather than relying on thirst signals that the medication has suppressed.
Injection vs. Oral — Why the Gut Experience Is Different
Subcutaneous injection of semaglutide produces significantly more consistent blood levels and a stronger gut effect than the oral tablet form. The oral bioavailability of semaglutide is approximately 1% — meaning the oral dose needs to be many times higher than the injection dose to produce comparable systemic levels, and even then, blood level peaks and troughs are more variable.
This variability in oral semaglutide means the gut effects can be more unpredictable — sometimes more pronounced around the time of peak absorption, sometimes less consistent throughout the day. People who have used both forms frequently report the injection form feels more consistent in both efficacy and side effect profile.
The oral form requires very specific administration — on an empty stomach, with no more than 4 ounces of plain water, at least 30 minutes before eating. Any deviation from this protocol significantly reduces absorption further. If you’re on oral semaglutide and feeling like it’s not working as well as expected, absorption protocol compliance is the first thing worth reviewing.
How Long Do GLP-1 Gut Side Effects Last?
This is the question everyone asks — and the honest answer is that it varies significantly by individual and by which side effect you’re dealing with.
Nausea is typically worst in the first 2–4 weeks after starting or after a dose increase, and improves meaningfully for most people within 4–8 weeks as the body adapts. Some degree of nausea with dose increases tends to repeat each time the dose goes up, then settles again.
Constipation tends to be more persistent — it’s driven by the ongoing mechanism of slowed colonic motility rather than an adaptation response. Most people need ongoing management strategies for constipation for as long as they’re on the medication at therapeutic doses.
Diarrhea in the early weeks typically resolves as the gut adapts, usually within 4–6 weeks. Persistent diarrhea beyond this deserves medical evaluation.
Acid reflux tends to persist as long as gastric emptying is significantly slowed — management strategies rather than resolution are the realistic expectation for most people.
Bloating typically improves as dose titration stabilizes and the gut adapts, but may persist at lower intensity throughout treatment.
The Complete Gut Support Protocol for GLP-1 Users
Based on everything above, here’s the practical daily protocol that addresses the full range of GLP-1 gut effects comprehensively:
With every meal — Digestive enzymes. Zenwise Digestive Enzymes — one capsule at the start of every meal. Compensates for disrupted enzyme timing, reduces post-meal bloating and gas, helps with fat digestion to reduce diarrhea risk. 👉 Amazon price here.
Daily — Quality synbiotic. Seed DS-01 — one dose daily. Maintains microbiome health through the transit time changes GLP-1 produces, supports immune function, reduces gas-producing bacterial overgrowth. 👉 Amazon price here.
Evening — Magnesium glycinate. Magnesium Glycinate 500mg before bed. Gentle motility support for constipation, improves sleep quality, supports smooth muscle function throughout the gut.
Daily — Psyllium husk. Psyllium husk capsules with a large glass of water. Normalizes stool consistency, feeds beneficial gut bacteria, provides prebiotic support alongside the probiotic.
Daily — Collagen peptides. Multi collagen peptides in your morning drink. Supports gut lining integrity during rapid weight loss, provides glycine for gut repair.
For nausea and motility — Iberogast. Iberogast drops before meals if nausea or slow emptying symptoms are significant. Prokinetic and antiemetic herbal formula with 60 years of clinical evidence.
Dietary Guidelines That Make the Biggest Difference
Small meals — always. Your stomach empties slowly. Overwhelming it with a normal-sized meal is the single most reliable way to trigger nausea, reflux, and discomfort. Think half portions or less at each sitting, more frequently through the day.
Protein first at every meal. Whatever you’re eating, eat the protein component first — before you fill up on anything else. On reduced caloric intake, protein preservation requires deliberate prioritization.
Low fat during difficult periods. Fat is the most powerful trigger for delayed gastric emptying amplification. During peak nausea periods or after dose increases, keeping fat intake low gives your stomach the best chance of emptying at a reasonable rate.
No eating close to bed. A stomach that empties slowly needs time. Eating within two to three hours of lying down dramatically increases reflux and overnight nausea risk.
Drink water on a schedule. Set a reminder if necessary. Aim for at least 8 glasses spread throughout the day — not with meals, which can worsen nausea, but between them.
Avoid carbonated drinks entirely. The gas they introduce into an already slow stomach significantly worsens bloating and nausea. Flat water, herbal tea, and diluted liquids are your best choices.
When to Contact Your Prescriber
Most GLP-1 gut side effects are manageable with the strategies above. But these situations warrant medical contact rather than self-management:
- Vomiting that prevents you from keeping food or medication down for more than 24 hours
- Severe abdominal pain — particularly upper left or upper central pain — that is new or unusual
- Signs of pancreatitis: severe persistent upper abdominal pain radiating to the back, with nausea and vomiting
- Signs of significant dehydration: dizziness, very dark urine, confusion
- Inability to eat more than tiny amounts for more than a week despite trying the management strategies above
- Diarrhea that persists beyond 4 weeks or is severe enough to cause dehydration
- Any gut symptoms that are getting progressively worse rather than improving after dose stabilization
Pancreatitis risk with GLP-1 medications is real though rare — severe abdominal pain while on these medications should always be evaluated medically rather than self-treated.
Frequently Asked Questions
Why does Ozempic/Wegovy cause so much nausea?
GLP-1 receptor activation occurs both in the stomach — slowing gastric emptying — and in the brainstem area that controls nausea and vomiting. The combination of a full-feeling, slow-emptying stomach and direct brainstem stimulation produces nausea in a significant proportion of users. It typically improves as your body adapts over 4–8 weeks.
Is constipation or diarrhea more common on GLP-1 medications?
Both occur, but constipation is actually more prevalent in clinical data — affecting 20–40% of users versus 8–15% for diarrhea. Constipation gets less attention because diarrhea is more immediately distressing when it occurs.
Can I take digestive enzymes while on semaglutide?
Yes — digestive enzymes are safe to take alongside GLP-1 medications and are genuinely useful for managing the bloating, gas, and post-meal discomfort that comes from disrupted enzyme timing and slowed digestion. Take them at the start of every meal.
Will a probiotic help with GLP-1 side effects?
Yes — particularly for bloating, irregular bowel habits, and gut microbiome disruption from altered transit times. A quality synbiotic provides ongoing microbiome support through the dietary and motility changes that GLP-1 medications produce.
How long do gut side effects last on Ozempic?
Nausea typically peaks in the first 2–4 weeks after starting or after dose increases and improves over 4–8 weeks. Constipation tends to persist throughout treatment and requires ongoing management. Acid reflux similarly tends to continue as long as gastric emptying is significantly slowed.
Does the oral pill cause more or fewer side effects than the injection?
Most clinical experience and patient reports suggest the injection produces more consistent side effect profiles — because blood levels are more stable. The oral form has variable absorption and may produce more erratic side effect patterns. The injection also tends to be more effective at equivalent therapeutic doses due to significantly better bioavailability.
Can I take magnesium for constipation on GLP-1 medications?
Yes — magnesium glycinate is one of the most appropriate interventions for GLP-1-related constipation. It works through smooth muscle support and osmotic water drawing rather than stimulant mechanisms, making it gentle and suitable for ongoing daily use.
Why am I so bloated on Wegovy even though I’m eating less?
Eating less reduces overall gut transit without eliminating bacterial fermentation — gas produced from what you do eat moves more slowly through a gut with reduced motility, accumulating throughout the day. Digestive enzymes reduce the fermentation substrate by improving food breakdown. A probiotic shifts the bacterial community toward less gas-producing strains. Both help significantly with GLP-1 bloating.
The Bottom Line — GLP-1 Medications Are Worth It, But Your Gut Needs Support
GLP-1 receptor agonists are genuinely remarkable medications. The weight loss outcomes for many people are transformative in ways that decades of conventional dieting never achieved. The cardiovascular and metabolic benefits beyond weight loss are substantial and increasingly well-documented.
But these medications work by fundamentally altering your digestive system’s operating parameters — and your gut needs active support to function well within those new parameters. Digestive enzymes to compensate for disrupted enzyme timing. A quality synbiotic to maintain microbiome health through altered transit. Magnesium and psyllium for constipation. Ginger and Iberogast for nausea and motility. Collagen for gut lining support during rapid weight loss.
This isn’t a complicated protocol. It’s targeted support for specific, predictable physiological changes. And for the many people who struggle with GLP-1 side effects enough to consider stopping — having the right gut support in place is often the difference between persevering and getting the results these medications can produce, and abandoning treatment before those results arrive.
Your gut can adapt. Give it the tools to do so.
More from TummyCure:
- Zenwise Digestive Enzymes — Full Review
- Seed DS-01 — Full Probiotic Review
- Magnesium Glycinate — Full Review
- Psyllium Husk Capsules — Full Review
- Iberogast — Full Review
- Multi Collagen Peptides — Full Review
- Turmeric Curcumin Gummies — Full Review
- Why Am I Always Constipated?
- Why Do I Feel Full So Fast When Eating?
- Why Do I Feel Sick After Eating?
- Diarrhea Every Morning Then Fine
- The Complete Gut Health Guide
About the Author
Rachel Donnelly is a certified nutritional health coach and gut health writer who spent years struggling with IBS and bloating before making digestive wellness her specialty. She writes for TummyCure with one goal: cut through the noise and tell you what actually works. When she’s not deep in microbiome research, she’s fermenting things in her kitchen and losing arguments with her husband about whether kombucha counts as a dessert.
As an Amazon Associate we earn from qualifying purchases through some links in our articles.





















