What’s with that constant urge to go—but nothing happens?
It’s one of the most frustrating feelings—you feel that pressure, like you really need to go, but when you sit down… nothing happens. Or maybe something barely happens, and you still walk away feeling uncomfortable, bloated, and annoyed.
I’ve been there more times than I’d like to admit. And let me tell you—it’s not just “in your head.” That constant urge to poop without results is often a sign that your gut, your muscles, or even your nerves are out of sync.
Sometimes it’s something physical—like stool that’s stuck or not quite ready to move. Other times, your body’s sending the wrong signals, reacting to inflammation, tension, or even anxiety. It’s surprisingly common, but it’s one of those awkward topics most people don’t talk about.
For me, it was happening enough that I had to figure out what was going on. Learning more about how the digestive system actually works helped me get past the frustration. If you’re in the same boat, TummyCure.com – Unlock the Secrets to Stomach Health is a solid place to start when everything feels off but nothing’s making sense.

Why do I feel like I need to poop but can’t?
This is the moment when your body’s like, “Go now!”—but then, you try and try… and nothing. It’s exhausting, uncomfortable, and it can mess with your whole day.
Common reasons this happens:
- Constipation
The most obvious culprit. Even if you sort of went earlier, there may still be stool sitting in the rectum causing pressure. - Gas buildup
I’ve had times where it wasn’t poop at all—it was just trapped gas. The bloating and pressure can feel exactly like the need to go. - Incomplete emptying
You go, but not all the way. That “unfinished” feeling sticks around and leaves your gut feeling confused. - Tight pelvic floor muscles
If your body’s tensing up or straining too hard, it might not be letting things move properly, even if you have the urge. - Inflammation or irritation
When your gut lining is inflamed (from IBS, infection, or even food sensitivities), it can send false signals that you need to poop—even when you don’t.
I used to think back pain had nothing to do with this, but when I learned about how pressure builds up across your gut and back, it made more sense. If this sounds familiar, Where Is Constipation Pain Felt in the Back? really helped me understand how much is actually connected.
What is tenesmus and what causes it?
If you’re constantly feeling like you need to go but barely anything comes out, there’s a name for that—it’s called tenesmus. I didn’t know that word for the longest time, but when I read about it, it described my experience perfectly.
So, what is tenesmus?
It’s the persistent feeling that you need to have a bowel movement, even when your bowels are empty. That uncomfortable pressure, the urge to push, and that “not done” sensation—it all falls under this umbrella.
Common causes of tenesmus:
- IBS (Irritable Bowel Syndrome)
Gut sensitivity and motility issues can cause lingering urges even after a full bowel movement. - Inflammatory bowel conditions
Things like ulcerative colitis or Crohn’s can irritate the rectum, triggering frequent false alarms. - Hemorrhoids or anal inflammation
Swelling in the rectal area can give off a constant “I need to go” signal—even when you don’t. - Infections or digestive upset
After a stomach bug or a flare-up, your gut might stay hypersensitive for a while.
I first read about tenesmus while trying to understand my IBS symptoms, and this article really helped: Chronic Diarrhea from IBS-D: Managing Symptoms and Hemorrhoids. It connected a lot of dots for me when I was feeling totally lost.

Can hemorrhoids or fissures make it hard to go?
Absolutely—and this was one of the things I had no idea about until it happened to me. At first, I just thought I was dealing with constipation, but it turned out I had a small fissure (tiny tear) and some hemorrhoid irritation. And even though my body felt like it needed to go, the discomfort made everything tense up.
How hemorrhoids and fissures mess with your bowel routine:
- Fear of pain = tension
When your brain knows pooping will hurt, your body may subconsciously tighten up the muscles down there—even when you’re on the toilet. - Swelling in the rectum
Hemorrhoids and inflammation can create a feeling of “fullness” or pressure, which tricks you into thinking you need to go. - Cramping and spasms
Rectal spasms can make it feel like something is there even if there’s no stool ready to come out. - Post-bowel irritation
Even after a full bowel movement, lingering inflammation or raw skin can keep that urge hanging around.
What helped me the most was learning how to soothe the area naturally and reduce the irritation. Effective Natural Remedies for Hemorrhoids You Can Try at Home became a go-to guide when I wanted to ease the discomfort without immediately turning to harsh creams or meds.

Is anxiety causing me to feel like I have to poop?
For me, the answer was a huge yes. I used to get this urgent feeling like I had to go—especially in the morning or right before leaving the house. Half the time, I didn’t actually need to poop. It was my anxiety triggering my gut into panic mode.
Why anxiety can make you feel like you need to go:
- Gut-brain connection
Your brain and digestive system are in constant communication. Stress can literally speed up or slow down digestion, and that miscommunication leads to confusion in your gut. - Fight-or-flight response
When you’re anxious, your body releases cortisol and adrenaline. That can cause stomach cramps, the urge to go, or even diarrhea. - Overactive vagus nerve
Anxiety can overstimulate the vagus nerve, which affects digestion and can give you a false poop signal. - Hyper-awareness of symptoms
When you’re anxious, you’re more in tune with every twinge or cramp, making the urge feel more intense than it actually is.
This is exactly why I used to wake up feeling off and rush to the bathroom—even when nothing happened. Why Does My Stomach Hurt When I Wake Up? helped me understand that stress and gut problems don’t just show up during big events—they can be part of your daily rhythm, too.

Could this be related to IBS or another gut issue?
When I kept feeling like I had to go but couldn’t, my first thought was constipation. But the more it kept happening—on and off, sometimes even multiple times in one day—I started wondering if it was something deeper. That’s when I learned more about IBS, and honestly, it explained a lot.
Why IBS messes with your urge to poop:
- Your gut becomes hypersensitive
With IBS, even a small amount of gas or stool can feel like your body’s screaming go now!—even when you don’t actually need to. - Incomplete emptying is common
Some days I’d go, but still feel like something was left behind. That “unfinished” feeling is part of how IBS throws off your normal gut rhythm. - Mixed-type IBS is extra unpredictable
I deal with the kind that swings between constipation and diarrhea, which makes the signals super confusing. One day I can’t go, the next day I can’t stop going. - Tension and bloating make it worse
When your gut is inflamed or full of trapped gas, it creates a phantom urge—like there’s something to pass, even if there’s not.
If your symptoms bounce between extremes and don’t seem to follow a clear pattern, it could be part of a broader gut cycle. I didn’t even know IBS could feel that inconsistent until I read this breakdown on managing both constipation and diarrhea without losing your mind. That helped me realize I wasn’t just imagining all the mixed signals.

Foods or habits that can make the urge worse
I started tracking what I ate and when the gotta go but can’t feeling hit me hardest—and sure enough, there were some clear patterns.
Triggers that made it worse for me:
- Greasy, fried food
These always left my stomach feeling sluggish and crampy, and weirdly made the urge feel stronger without results. - Dairy products
Even though I’m not fully lactose intolerant, dairy often left me bloated and triggered that uncomfortable pressure. - Caffeine overload
Coffee used to be part of my morning routine, but it started making things worse—lots of urgency, very little action. - Holding it in too long
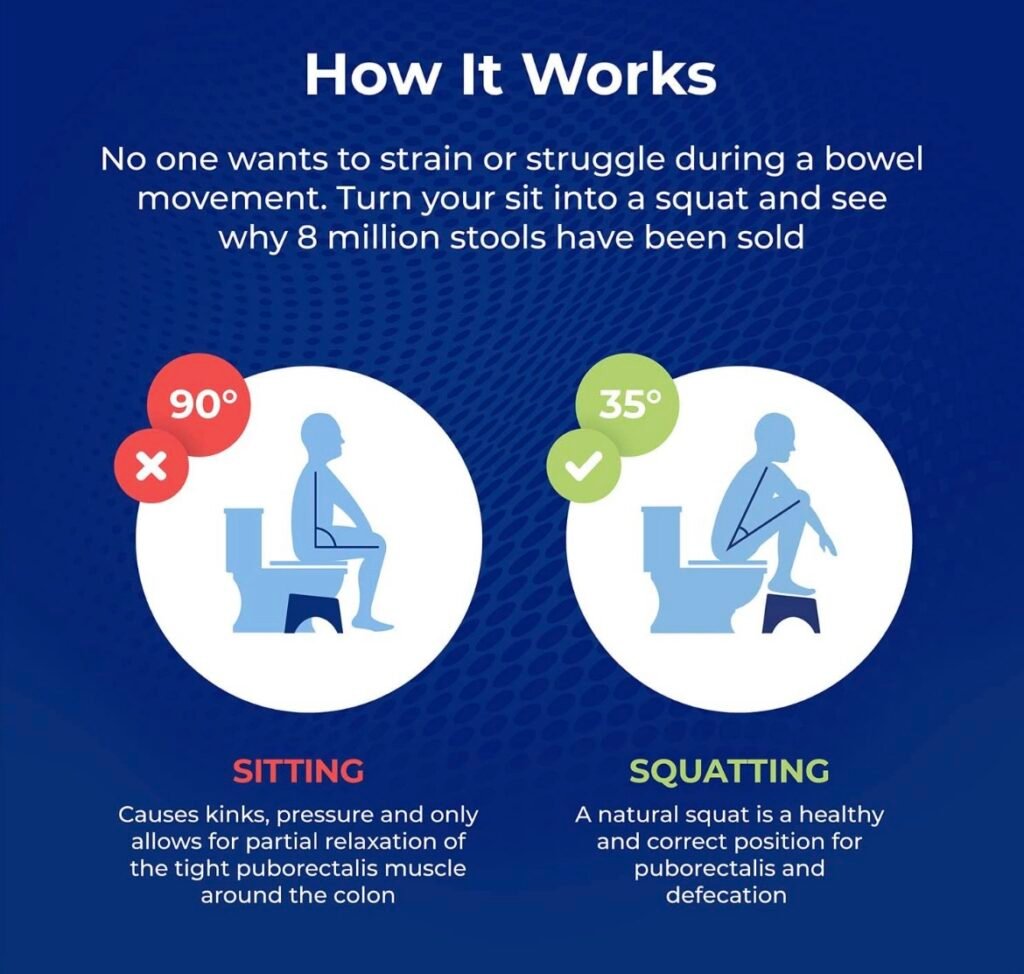
Life gets busy, and I’ve ignored the urge more times than I’d like to admit. That just leads to mixed signals and straining later. - Bad bathroom posture
Once I switched to a better sitting position (yep, I finally tried a squatty potty), things felt smoother and less forced.
I also noticed that when my stomach felt unusually tight, bloated, or just heavy, the incomplete urge was stronger. If that’s happening to you too, this article on ways to ease that sluggish, bloated gut feeling lays out a few tricks that made a difference for me—especially when I needed to get things moving without overdoing it.

What helped me when I couldn’t go but felt like I had to
When that stubborn urge wouldn’t go away, I had to experiment with a bunch of different things before I found what actually worked for my body. It wasn’t always about going harder or trying to “force it”—sometimes it was about helping my gut relax and get back into rhythm.

Here’s what actually helped me feel better:
- A slow walk around the house
Gentle movement made a huge difference. Even just pacing for 10–15 minutes helped reduce the pressure and ease cramps. - Warm compress on my belly
When I felt bloated and stuck, heat worked better than anything else. I’d lay back with a warm rice sock and let my gut calm down. - Upping my hydration
I started sipping more water throughout the day (especially warm or room temp), and it helped everything move more regularly—without the sudden urgency. - Switching to calming teas
Peppermint and ginger tea became part of my routine. They soothed my stomach and helped things pass more naturally. If you’re looking for something to try, these herbal teas made for gut relief were honestly a game-changer. - Breathing and posture
I never realized how much I clenched my stomach and pelvic floor until I made a conscious effort to breathe deeper and sit in a better position. That simple shift helped my body stop fighting itself.
Sometimes the solution wasn’t getting my body to “go,” it was getting it to stop panicking long enough to let things work naturally.

When to talk to a doctor about the urge with no results
Look, I’m all about figuring things out at home, but if that constant “I need to poop” feeling just won’t go away, there’s no shame in asking for help. I waited way too long, and I wish I had spoken up sooner.
Signs it might be more than just occasional constipation:
- The urge happens daily or multiple times a day
- You’re in pain or straining with no results
- You notice blood, mucus, or odd changes in your stool
- You’re losing weight without trying
- You feel exhausted or dizzy after every bathroom attempt
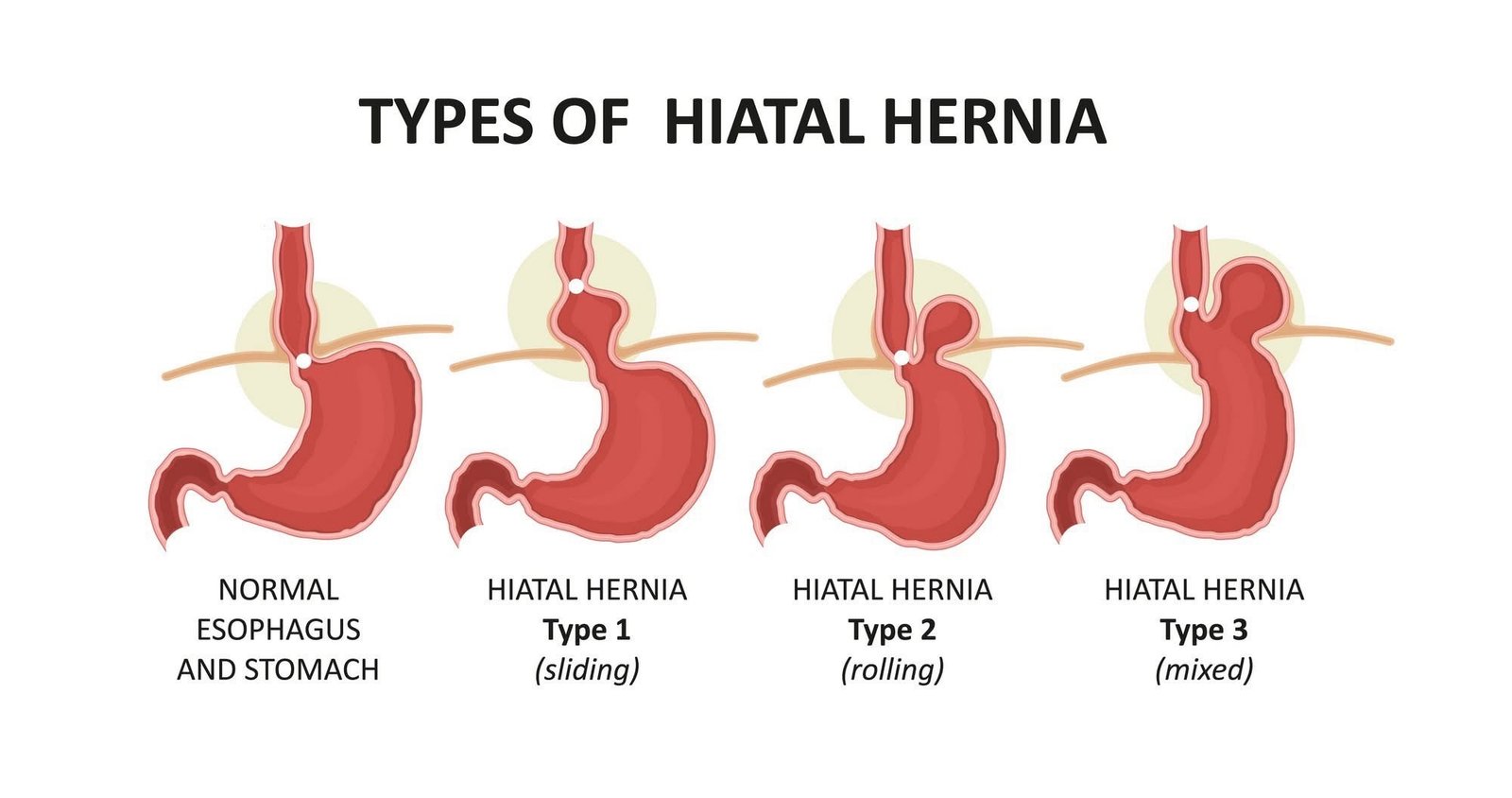
In my case, things started to improve once I ruled out anything serious and focused on calming my system down. But if the urge is constant or keeps coming back in cycles, your doctor might check for IBS, inflammation, rectal issues, or even a hernia.
I remember worrying about what I’d do if I needed something like surgery—but this guide on understanding hiatal hernia costs and care gave me some peace of mind when I was Googling worst-case scenarios at 2 a.m.
If this is happening to you, know this: you’re not crazy, and you’re not alone. It’s frustrating, but your body’s trying to tell you something—and with a little help, it will get easier to understand.

As an Amazon Associate we earn from qualifying purchases through some links in our articles.